Not sleeping but not sleepy with asymptomatic apnea
As many as 25% of apnea sufferers don't complain of daytime sleepiness. Compliance is a problem because these patients may not see the value of treatment, according to researchers at the American Thoracic Society.
NEW ORLEANS—Usually in a discussion of treatment options, the patient has questions and the doctor offers the answers. However, during the session “Should we treat asymptomatic obstructive sleep apnea patients?” at the May meeting of the American Thoracic Society (ATS) in New Orleans, the only speaker with a definitive answer was the patient.
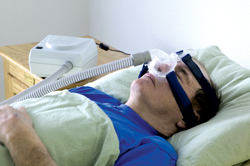
“My answer is yes,” said Michael Goldman, a corporate lawyer who had experienced no problems with daytime sleepiness before being diagnosed with sleep apnea. Yet treatment with continuous positive airway pressure (CPAP) changed his life. “It's just like a fog I didn't even know existed has been lifted,” he said.
The sleep apnea researchers who spoke during the session were less enthusiastic about the benefits of treating asymptomatic patients, whom they defined as those who don't complain of daytime sleepiness. The main problem is that there are so many of them. Studies have estimated the prevalence of sleep apnea as high as a quarter of the population.
“If we want to treat all these patients, we have a lot to do,” said Malcolm Kohler, MD, of the University Hospital of Zurich in Switzerland.
It's also unclear what benefits the patients will receive from treatment. A number of studies have tried to determine whether CPAP treatment reduces cardiovascular risk in patients who aren't sleepy. But it's difficult to draw definitive conclusions, Dr. Kohler said, because the evidence of an association with cardiovascular events comes from cohort studies, while most of the controlled studies looked only at surrogate markers.
Some additional data on the question were presented at the ATS meeting by a group of Spanish researchers. The trial included 724 non-sleepy patients randomized to CPAP or conservative treatment (advice on weight control and sleep). Treated patients were less likely to have cardiovascular events and hypertension. “We need to treat 32 patients with CPAP to avoid one new event,” said study author Ferran Barbé Illa, MD, of the Hospital Arnau de Vilanova in Spain.
However, the effect only reached statistical significance among patients who used their CPAP machine for at least four hours per night. Compliance tends to be a problem among these patients, noted Teri Weaver, PhD, RN, of the University of Pennsylvania in Philadelphia. Less sleepy patients are less likely to stick with CPAP, likely because they perceive less benefit.
“It may not be sleepiness itself but how sleepiness affects daily activities,” she said.
Daily functioning
The significance of sleepiness to daily functioning is a complicating factor in addressing sleep apnea in the elderly, who tend to have a higher prevalence of sleep-disorder breathing, but lower scores on sleepiness scales. “Older people have an increased opportunity to nap,” noted Mary J. Morrell, PhD, of the Imperial College School of Medicine in England.
The breathing problems of the elderly are hard to separate from comorbidities, but even super-healthy elderly patients have been shown to have breathing issues during sleep, possibly due to structural changes to the airway, Dr. Morrell said.
One study that used mortality as an outcome even found that moderate sleep apnea could be protective—patients who had it were actually less likely to die than those without. “It presents more questions than answers,” said Dr. Morrell. “There are potential cardiovascular consequences but I don't think there are enough data on it [in older people] yet.”
She hopes to have more data within the next few years, having just received funding to conduct a large trial of sleep apnea in elderly patients in the United Kingdom.
Assessing risk
Cardiovascular effects are not the only reason to treat sleep apnea, however. “Patients with obstructive sleep apnea are more likely to have motor vehicle crashes than normal individuals,” said John A. Fleetham, MD, of the University of British Columbia in Vancouver, Canada.
The risk appears to apply just as much to patients who say they are not sleepy. “There's no clear pattern with crash rate being associated with Epworth sleepiness scale,” he said.
In fact, patients who don't think they have daytime sleepiness could potentially pose more risk, because they are unaware of their sleepiness. Another potential issue is that patients may misrepresent their sleepiness to avoid consequences like losing their drivers' licenses.
Physicians treating these patients are put in the awkward position of having to balance public safety with a patient's individual benefit and wishes. The decision on how to treat the patient and whether to report him or her to authorities rests on relevant local law, which is “all over the map,” according to Dr. Fleetham. “Be aware of the motor vehicle legislation according to your local area,” he advised.
On a societal level, he has concerns about requiring doctors to report patients with sleep problems. “Such reporting may discourage many drivers from seeking treatment,” he said.
On an individual level, he bases his decisions on patients' attitudes, such as whether they agree to not drive when sleepy, and their driving habits. CPAP treatment is a priority for commercial drivers with apnea, for example.
Official guidelines from a 2006 joint task force of the American College of Chest Physicians, American College of Occupational and Environmental Medicine and the National Sleep Foundation call for taking commercial drivers off the road prior to further assessment if they have an Epworth sleepiness scale of 16 or more, but there's not much evidence to support that cutoff, according to Dr. Fleetham. “I was amazed by how little data there is,” he said.
It was a theme repeated throughout the session: Experts in the field are not ready to answer the question posed by the session title, even after years of study. Dr. Weaver noted that she also spoke on the subject at the 2001 ATS meeting. “I could still use the same slides,” she joked.