New research links empathy to outcomes
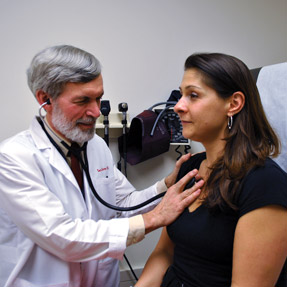
Everyone wants to have a physician who understands what they're feeling, but it's not just about human contact; better clinical outcomes can result from physician empathy.
It's not hard to understand why patients might value empathy in medicine.
“Who doesn't want to have a physician who understands what they're feeling? Everybody wants that. Everybody feels in their gut that is important,” said Daniel Z. Louis, managing director of the Center for Research in Medical Education and Health Care at Jefferson Medical College in Philadelphia.
But Mr. Louis and his colleagues suspected that the benefits of empathy extend beyond good feelings, and they recently found evidence for it in a study of 242 Italian primary care physicians and 20,961 diabetic patients.
In the study, which was published in the September 2012 Academic Medicine, patients whose physicians scored highly on a empathy test had significantly fewer acute diabetes complications, such as diabetic ketoacidosis, than those whose physicians were less empathic.
The association of empathy with a patient outcome, in a fairly sizable population, was a significant breakthrough. “We put it to the most difficult test,” said Joseph S. Gonnella, MD, a study coauthor and dean emeritus at Jefferson. “We are confident in what we have found.”
Now they and other researchers will move on to the other effects empathy might have on patients; why; and, most important and most difficult, how to mint and maintain empathic physicians.
At the start
The whole field of empathy research is relatively new. It was only a couple of decades ago that experts began by defining empathy, especially in contrast to sympathy, with which it is often confused.
“It involves an attempt to understand the patient as opposed to an attempt to feel for the patient, which is sympathy. A capacity to communicate this understanding combined with an intention to help is part of the definition,” said Mohammadreza Hojat, PhD, a study coauthor and professor at Jefferson and author of “Empathy in Patient Care: Antecedents, Development, Measurement, and Outcomes.” An empirical study by Dr. Hojat and colleagues suggests that empathy in the context of patient care includes three underlying components: perspective taking, compassionate care and walking in the patient's shoes.
Despite this conceptualization, physicians can have very different, yet successful, approaches to empathy, noted Jodi Halpern, MD, PhD, author of “From Detached Concern to Empathy: Humanizing Medical Practice.” “There are empathies, not just one kind of empathy,” she said. “It's not like everyone has to do it the same way.”
Curiosity is an important component, she noted, and not just the kind that leads you to order a CT scan. “It has to be grounded in concern or respect for [patients]. It's not just treating somebody as a curiosity,” she said. “There's a complexity to each person's experience that should make us genuinely interested.”
A little more than a decade ago, the Jefferson researchers quantified these qualities in a questionnaire that could be administered to physicians and medical students. The Jefferson Scale of Empathy contains 20 statements that measure a clinician's empathy, such as “My patients feel better when I understand their feelings,” “I consider understanding my patients' body language as important as verbal communication in physician-patient relationships,” and “Because people are different, it is almost impossible for me to see things from my patients' perspectives.”
Despite even its authors' initial doubts (“I was very skeptical about trying to document the presence of empathy using a paper and pencil,” said Dr. Gonnella), the scale has been validated in many studies and translated into 43 languages.
With a measurement tool established, researchers began assessing the levels of empathy around them. Their findings were concerning, and somewhat counterintuitive.
“Empathy declines during the course of medical education among students as well as residents. This decline happens in the third year of medical school, the year that students are formally involved in patient care,” said Dr. Hojat. “You expect a different pattern, that their attitudes toward patient care and empathic engagement would improve.”
The finding naturally raised concerns among medical educators. “We take a normal human first-year medical student who is going to be concerned and curious about patients. What are we doing to ruin it?” asked Dr. Halpern.
Explaining the drop
Experts have theories about the possible causes of the decline in empathy.
“Sometimes students are overwhelmed by the nature of clinical medicine. They are, for the most part, still very young human beings who are confronted with death and dying and suffering and conflict,” said Johanna Shapiro, PhD, director of the program in medical humanities and arts at the University of California, Irvine School of Medicine.
The doctors-in-training might also hold traditional beliefs about the value of physician detachment. “The same doctor that might have lots of curiosity and concern about people outside comes into the hospital with the baggage, ‘I'm a doctor. I'm supposed to be a scientist and detached,’” said Dr. Halpern. “That's not true ... I work with nurses and social workers and they're not trained that way. They have just as many emotionally difficult situations.”
Additionally, there's the nature of the modern clinical encounter. “It's tough to be empathic when you have five minutes with each patient. It's tough when the patients are not pleasant,” said Mr. Louis.
But, on the bright side, empathy can actually make it easier to deal with those hard patients. “When you're seeing a diabetic patient for the 20th time and their hemoglobin A1c is going up, of course you're going to be frustrated. You're not going to be empathic initially,” said Dr. Shapiro.
The key is to acknowledge that feeling and also the necessity of having empathy for that patient. “When we become aware of our emotions we can shift them a little bit,” said Dr. Shapiro, who talks to students about remembering that every patient is someone's parent or child. “Instead of inadvertently belittling the patient in small but unmistakable ways, the student can express interest and curiosity by asking the patient, ‘What's going on?’”
Empathy exercises
Analyzing one's emotions is one of the simplest empathy improvement tools offered by the experts.
“If physicians regularly take time to reflect on their practice and patient care, they can in a sense be refreshed and reminded of the important role they have in patients' lives,” said Daniel Chen, MD, assistant professor and associate clerkship director for internal medicine at Boston University.
This reflection could take the form of journaling. The “On Being a Doctor” and “A Piece of My Mind” sections of Annals of Internal Medicine and the Journal of the American Medical Association, respectively, demonstrate this kind of reflection. “These essays are very rich in empathy. When it's documented in such a public venue it validates something that we should be doing,” Dr. Chen said.
Some training programs have incorporated this practice. “We have each student write a clinical narrative about something that caught their attention, bothered them, reaffirmed their reason for being in medicine” at the end of their internal medicine rotations, said Dr. Chen.
The students then discuss these experiences, another practice that can build empathy in training and practicing physicians. “If there's a case or a patient that is challenging, that exhausts a person, very often colleagues will talk, often under the guise of ‘I just want to vent,’” said Dr. Chen. If the venting, formal or informal, leads to reflection on how the interaction could have gone better or how the patient might have felt about it, it could potentially improve empathy.
With students, educators have tried some more dramatic ways to convey patients' feelings. A Jefferson project assigned students to shadow patients admitted to the emergency department. “We administered the Jefferson scale pre- and post-experiment and we noticed the empathy score in those who shadowed the patient did not decline, but in the control group, their empathy score declined,” said Dr. Hojat.
In another trial, the researchers had students wear glasses covered in Vaseline, plug their ears and use a walker to simulate life as an elderly person. “Those who were exposed to this kind of experiment for one hour, their score increased immediately,” Dr. Hojat said.
It would seem like a promising solution to the decline in empathy during training, except for one problem. “A few weeks later, when we administered the scale again, it went back to the original,” he added.
Later reinforcement, such as a lecture repeating the learned concepts, has shown some promise for maintaining empathy, although it's not certain how often that would be necessary. “Maybe periodically all of us should be hospitalized. Having somebody be quadriplegic will do much more than a lecture or a role model,” said Dr. Gonnella.
Models needed
Empathic role models could still make a big difference, however, the experts said.
“Sometimes students are frustrated because we talk at them all the time about how important these things are and then in practice, they don't see the same level of consistency,” said Dr. Shapiro. “Once they reach the clinical years, they are rarely asked, ‘How do you think your patient is feeling?’ or ‘How do you think your patient understands this situation?’”
Older physicians could also potentially help learners by teaching and modeling behaviors that are typically associated with physician empathy, although this area is under some debate. “To feel empathetic, yet not be able to demonstrate it, is that better than not having as much empathy but being able to give the appearance?” asked Dr. Chen. “I don't know.”
His research, comparing student surveys with mock patients' assessments, has hinted at the existence of a divide between how physicians view their own empathy and how patients see it. “Although the students from second year to third year reported a decrease in self-reported empathy, they were able to demonstrate to the patient more empathy,” he said.
What appeared to the patients to be more empathy was probably the result of education on communication techniques. “We're teaching our students to always wait until the patient's done speaking, use facilitating words, even the nitty-gritty of body posture,” said Dr. Chen.
These techniques are not the same as empathy, but they might be a helpful step toward achieving it, according to Dr. Shapiro. “It's kind of like Method acting,” she said. “A behavioral approach to empathy can be beneficial in that it gives students who are feeling overwhelmed in clinical situations anchors to hold on to.” But, she added, behavioral techniques should be the beginning, not the endpoint, in developing empathy.
Some tricks for when one is feeling overwhelmed can help experienced physicians maintain their empathy, too. Solutions can be as simple as counting to 10 or as intensive as studying meditation or mindfulness.
The latter options are more time-consuming, of course, and as with any improvement to the medical visit, the time crunch is a major obstacle. “If a provider has limited time for the encounter, he may not have time to effectively communicate his understanding back to the patient, even though he may understand,” said Dr. Chen.
Feeling out the future
However, the new findings on the effects of empathy, from the Italian diabetes study, could change the equation. The Jefferson researchers concluded that based on their results, “empathy should be considered an important element in patient care and a significant factor of overall physician competence that must be enhanced during medical education, and applied in the practice of medicine.”
In other words, empathy may have significant enough effects to grab some of physicians' limited time. First, though, the researchers need to figure out how to best use that time to patients' benefit. “What is the cutoff point [for an acceptable empathy score]?” asked Dr. Gonnella. If a cutoff were set, decisions about physician hiring, medical school acceptance or the need for empathy training could be based in part on empathy scores, he added.
The cutoff might be different for different specialties, Dr. Hojat noted. “When we administered this to a large group of physicians, and we compared their scores, we found that family practitioners, general internists, pediatricians and psychiatrists obtained the highest scores,” he said. Empathy might turn out to be less critical for technology-oriented specialties, such as pathology, radiology or anesthesiology.
Whether those primary care specialties attract more empathic people or teach them more empathy is a question along the lines of whether the chicken or egg came first, said Dr. Chen. But it's one that researchers might need to investigate if they're going to maintain our supply of both primary care physicians and empathic doctors.
In Dr. Chen's case, one of those medical student lessons in empathy, an essay-writing assignment, convinced him to enter the empathy-oriented specialty of internal medicine. “I had the grades and the scores to do ortho. But ... after writing the essay, I realized there's a richness to be experienced in internal medicine,” Dr. Chen said.