Programs start early to promote health careers
Rural facilities are recruiting their next generation of doctors early##mdash;from high school. They're offering paid, entry-level jobs to immerse the youngest scholars in a health care environment with the hope they'll pursue careers in the field.
Obstetrician Eric Fish, MD, had a lot to do when he first began working at Schneck Medical Center in Seymour, Ind. “My day consisted of mowing the grass, planting flowers, picking up cigarette butts, whatever needed to be done,” Dr. Fish said.
Of course, these tasks are not typically assigned to physicians at Schneck. Dr. Fish first worked for the hospital just after his high school graduation, when he had interest in a health care career and a need for a summer job.
His hometown hospital provided him with not only employment for multiple summers, but also scholarships toward college and medical school tuition and, when he was ready to decide on a medical specialty, shadowing and moonlighting opportunities with various departments.
The hospital's generosity is motivated by a desire to attract physicians to this rural facility, explained Mindy Roeder, Schneck's director of physician recruitment and administrator of the hospital's “Grow Our Own” program. “Someone from our area is more likely to come back,” she said.
Her conclusion is supported by the evidence, according to researcher Howard K. Rabinowitz, MD, a professor of family medicine at Jefferson Medical College in Philadelphia. Some urban natives are recruited to combat the rural physician shortage, “but mostly it's people who grew up in small towns and rural areas,” he said.
Hospital administrators and educators have noticed this dynamic, and it's led them to focus some recruitment efforts on potential employees who may be thinking more about passing notes than passing boards. Several programs in different parts of the country are working to introduce high school students to health care careers.
An early start
Starting recruitment so early has not been the traditional strategy for rural leaders, noted Kathleen Quinn, PhD, program director of the University of Missouri's Area Health Education Center.
“Legislators concentrate more on rural training tracks at the residency level,” she said. “Loan repayment programs get tons of money.”
But residency may be too late to attract suitable candidates to rural practice, according to research. For one thing, the needed number of small-town natives may not make it to that point in the process on their own.
“It's a bit overwhelming, the years of training, the huge debt obligation, especially if they don't have a lot of family support,” said Dr. Rabinowitz. “A lot of people just don't even think about it.”
The high school programs aim to correct that. “We try to give some hope to kids that maybe never thought about the fact that they could become physicians,” said Patricia J. Stubber, executive director of the Northwest Pennsylvania Area Health Education Center (AHEC).
Pennsylvania's AHEC program includes education for younger members of the health professions pipeline. It educates youngsters about health care careers, organizes shadowing opportunities and runs summer camps focused on health care careers. The program can't reduce the time and money required to become a physician, but it can try to change kids' perceptions of these obstacles.
“They think being a physician is totally out of their reach. They think a lot of it is financial, which it is, but there are means to address that,” said Ms. Stubber. “We can direct them to financial resources.” Some programs, such as Schneck's, offer direct financial assistance, while others direct students to possible sources of grants and loans, including medical societies, government programs and the schools themselves.
Skill-building
By starting in high school, the programs can also help ensure that students are academically prepared to go into health care.
“We want them to start thinking about careers so that they can make some good decisions about not only their courses of study, but also about good study habits, getting good grades and looking into the right kinds of further education or job opportunities,” Ms. Stubber said.
Academic preparation is a major component of the Louisville Trover Campus' High School Rural Scholars Program in Kentucky. The program is aimed specifically at students who appear to need the assistance, such as those who are interested in medicine but don't have the highest ACT scores, according to William Crump, MD, associate dean of the campus.
“These are the kids that are on the cusp,” he said. This group might go to medical school, or become nurses or nurse practitioners, but they are also in danger of giving up on a medical career entirely.
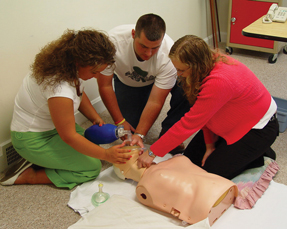
For these students, the program provides a summer of free ACT tutoring, led online by instructors from local colleges. The tutoring is conducted over the Internet because keeping these rural students in their hometowns is a major focus of the program.
“There are lots and lots of programs that take bright young kids and take them to the big city,” said Dr. Crump. “If you take them to a medical center or an urban environment, the message is clear: To do something really special in medicine, you need to go to these places. Well, that's antithetical to what we're trying to do.”
The Trover program arranges for the students to shadow health care professionals in their hometowns. The various programs for high schoolers vary in the extent to which they focus on medicine specifically versus health careers in general.
“In addition to physicians, we have them shadow physicians' assistants, nurse practitioners, dentists, veterinarians, pharmacists, physical therapists and occupational therapists,” said Dr. Crump. “These are rising high school seniors. They don't know what they want to do.”
The hope is that the shadowing experience will help the students refine their career plans. It also provides them with the equivalent of a summer job. “These kids have to work. They can't take six weeks off,” said Dr. Crump. “That's why we pay a stipend that's the equivalent of minimum wage.”
Regardless of whether the programs pay the high schoolers, they provide some real-world experience that can be useful later on, such as during pre-admission interviews.
“They'll be able to talk about the health care profession better than someone who's gotten their information from television or limited experience,” said Robert Bennett, PhD, associate professor of internal medicine at the University of Nebraska Medical Center (UNMC) and a faculty member of the UNMC High School Alliance.
The alliance is a particularly ambitious effort. It pulls juniors and seniors from local high schools to the medical center for a year-long academy. Every afternoon, the students are taught by UNMC faculty members about various pre-medical subjects, including anatomy, genetics, infectious diseases and pathology.
The classes may be tailored to a high school audience instead of pre-med students, but they provide new challenges to the instructors, according to Dr. Bennett.
“It's good to have to get out of your comfort zone and think of new and creative ways to present the information,” he said.
Volunteer labor
The willingness of Dr. Bennett and others to contribute their time and expertise is the foundation of all of these efforts. “Just having a physician champion in their lives, we've identified as a very important thing that we do,” said Ms. Stubber.
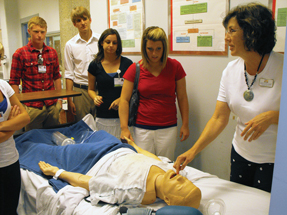
At Schneck, where Dr. Fish got his start, the offerings for high school students include evening programs during which physicians explain their work to groups of interested kids. For example, a surgeon and an anesthesiologist have shown video of laparoscopic surgery, and an obstetrician brought in a pregnant patient and let the kids perform an ultrasound.
“Our physicians are gracious enough to volunteer their time,” said Ms. Roeder.
In Kentucky, each community has a coordinator who recruits volunteer clinicians to be shadowed. “Because these kids are from their own communities, they already know most of them,” said Dr. Crump. “The local shadowing coordinator doesn't have any trouble finding [clinicians] that are enthusiastic.”
Of course, not every clinician is eager to recommend a career in health care. “We have had some kids come through and say, ‘I spoke with a doctor and they told me if they had to do it over again, they wouldn't do it,’” Ms. Roeder said.
Not surprisingly, the program coordinators try to avoid connecting students with mentors who are unhappy in their careers. But they do want the kids to get a realistic view of working in health care, even if some of them are scared off by it.
“The 25% that don't end up in health careers, those go in the win column also, because I've seen too many bright kids get two, three, four years down the pipeline and think, ‘I don't want to do this. I can't deal with warm, smelly people,’” said Dr. Crump.
As his statement implies, the Kentucky program has found in its first 12 years that about 75% of its graduates go on to further training in health care. The Schneck program doesn't keep track of percentages, but Ms. Roeder reports that 16 physicians later practiced at the hospital after being targeted for recruitment as youngsters.
The Nebraska alliance plans to follow its alumni, but since it's only in its second year, administrators don't know yet whether the classes and clinician shadowing program will lead students into health care careers.
“About 90% walked in knowing that they want a career in health somewhere. Others were testing the waters,” said Ashlie Nelson, a high school teacher in the academy. “By the time they left, we had a couple of successful stories where students realized that health science was not for them.”
Loading the pipeline
It's likely that more students will drift away as they move through the health care training pipeline.
“The pipeline itself isn't straight across,” said Dr. Rabinowitz. “It gets narrower. If you take 100 people who are interested in medicine in high school, the number who become physicians is actually much smaller. If you take the number [of interested people] entering college, it's better.”
For some rural schools and communities, it's worth taking that gamble.
“UNMC is doing this because they want to address the health care employee shortage that we've all read about, all the way from nursing to physicians and everywhere in between,” said Heidi Kaschke, program coordinator. “If we can expose students when they are in high school to these opportunities, it might help bridge those gaps.”
Dr. Fish certainly believes in the system. Not only has he held numerous positions at his hometown hospital, but his wife, a physical therapist who didn't grow up in the area, was recruited to work there as well.
“For us, meeting the people at Schneck, seeing how they care about the organization, they care about the community, it just really made you want to come back,” he said. “I think smaller rural community hospitals need to be in tune with who is there in the community.”





