Build your own ultrasound-guided thoracentesis simulator
The use of bedside, portable diagnostic ultrasound devices by nonradiologists is increasing, because of both maturing, more affordable technology and evidence supporting improved patient safety and process efficiency.
The use of bedside, portable diagnostic ultrasound devices by nonradiologists is increasing, because of both maturing, more affordable technology and evidence supporting improved patient safety and process efficiency.
Hand-carried, battery-powered, high-quality ultrasound machines are now available at a small fraction of the costs of conventional technology. With minimal training, hospitalists, critical care clinicians, emergency physicians, and internal medicine residents have been shown to achieve competence in focused, brief, urgent and goal-directed sonographic applications such as:
- procedural guidance (arthrocentesis, paracentesis and thoracentesis),
- assessment of cardiac ventricular size and function in urgent and emergent settings,
- central venous pressure assessment and
- pneumothorax assessment.
Relying exclusively on physical examination and clinical assessment for these questions exposes patients to avoidable transfers, delays of care, inappropriate interventions and therapies and long wait times in diagnostic departments. Ultra-sound is superior to chest X-rays in determining the presence and location of pleural fluid, and ultrasound guidance is associated with a lower pneumothorax risk (<1% to 5%).
Training residents and physicians to use ultrasound for a procedure such as thoracentesis can be expensive from the standpoint of simulation technology. Many institutions now have portable ultrasound devices available to educators; however, lack of access to simulation models can present a stumbling block to training. Several very good simulation models include internal effusions for aspiration, but these can cost thousands of dollars for a single model.
Handheld ultrasound simulators can be reproduced in any training environment, practice group or at home as a very workable alternative to commercial models and for a small fraction of the cost. Both methods provide high-fidelity images and an authentic procedure experience. The do-it-yourself model does require more prep time in terms of setup and cleanup but much lower capital costs. Basically, it's the cost of a rack of pork ribs.
Supplies for the simulation:
- a utility knife,
- a magazine filing box or shallow cardboard book shipping box (Physicians' Desk Reference works well),
- 1-gallon sealable plastic bag,
- tape,
- half-rack of pork spare ribs (preferably with parietal pleura attached) and
- twine or zip ties to attach ribs to box
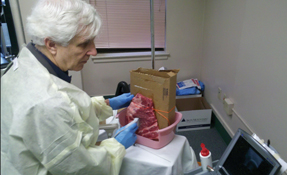
Instructions for construction:
Step 1. Using a utility knife, cut a 10- to 15-cm square out of the flat/face side of box.
Step 2. Fill plastic bag with water so that it is relatively firm when sealed.
Step 3. Slip plastic bag into the cardboard box and tape up the box.
Step 4. Place ribs parietal pleura side down (against the fluid-filled bag) and secure them to cardboard box using twine or zip ties. Side of plastic bag should protrude slightly beyond the plane of the box wall.
The box with ribs attached should be elevated on some kind of semi-vertical stand if you intend to simulate the procedure on a seated patient. Conversely, the simulation model should be laid flat to simulate a supine patient.
Thoracentesis procedural checklist:
- Position patient as normal, seated upright vs. supine (ventilated).
- Determine whether there is fluid. (Scan dependently.)
- Map extent of fluid in two planes.
- Note proximity of lung, heart, liver, spleen, and diaphragm through respiratory cycle.
- Mark needle entry site (above rib to avoid neurovascular bundle).
- Prepare site with chlorhexidine or povidone-iodine.
- Anesthetize and aspirate.
Suggested teaching format
A typical ACP Clinical Skills workshop will consist of presenting introductory educational content, some faculty demonstration, and ample time for participants to practice the procedure or examination skill with feedback from the faculty.
The workshop should be scheduled to run at least a half-day and should be organized with an assumption of three to four participants practicing on a model and one instructor supervising/providing guidance for each small group.
A suggested format for a workshop would be as follows:
1. Begin with didactic presentation (ultrasound basics: image acquisition, probes and basic “knobology”).
2. Practice imaging anatomy of participants/volunteers. Nonphysician sonographers are often pleased to be involved.
3. Practice performing the procedure (with direct faculty observation, guidance and feedback).
4. Summarize the information provided and offer a chance for Q&A.
After the simulation is completed, cleanup involves disposal of the pork ribs. See sidebar “Cleaning up” for a recipe for this process.