Medical missions in Iraq help train next generation of doctors
U.S. military physicians are helping to train Iraq's next generation of doctors, as well as helping to restore an infrastructure smashed by decades of neglect then the shock and awe of combat.
Iraq's national medical community suffered both under its pre-war regime and the subsequent war and looting that destroyed infrastructure and led senior physicians to flee the country, leaving few experienced professionals to train the next generation of doctors.
The U.S. Army is using its medical expertise to try to improve the situation. Through the Over the Shoulder program, a collaborative effort between the U.S. State Department, the Department of Defense and the Iraqi Ministry of Health, recent Iraqi medical school graduates spend two weeks shadowing and assisting U.S. physicians as they go about their regular duties at the Ortiz Troop Medical Clinic at Forward Operating Base Prosperity in Baghdad.

The program is part of the U.S. Provincial Reconstruction Team's work, which began in 2005. (A military-produced video about it is online.) ACP Fellows Lt. Col. Edward McDaniel, MD, and Major Ahmad Slim, MD, have participated.
Dr. McDaniel, an internist, worked in the program from July 2010 to January 2011. He is a 16-year Army physician whose time with the Over the Shoulder program took place during his second deployment to Iraq. Dr. Slim, a cardiologist, took over from January 2011 until he rotated out of Iraq in June. Both are career military doctors stationed at Brooke Army Medical Center in Texas.
Both doctors described the physicians they worked with as the cream of the crop of Iraq's recent medical school graduates. Participants, who serve two at a time, have included men and women, and one session hosted a husband-and-wife team. Several dozen physicians have completed the program and there is a waiting list for future slots. Participation is open to any Iraqi doctor who is willing to venture into the international zone, which requires driving through extensive security checkpoints, taking up to two hours each day.
“They had to get up at 4 a.m. in order to be on the post by 8 each morning, and they were literally risking their lives to get there,” Dr. McDaniel said. “You have to be very motivated to go through that.”
What participants learn
Once inside, the participants, all of whom speak English well enough to not need a translator, shadowed the U.S. physicians through everything from basic examinations for back pain to major trauma situations, with patient permission.
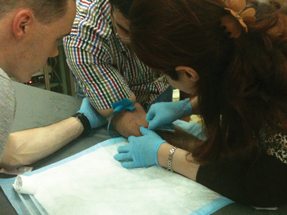
“They get hands-on experience doing things like inserting a central line, performing ultrasounds, intubating patients and resuscitating trauma victims,” Dr. Slim said. “Many of them have never had the opportunity to do these things before, not only because there are so few people to train them, but also because supplies are scarce.”
The participants rotate through a wide range of areas, including the laboratory, radiology, behavioral health and dentistry. They also learn about operational issues, such as the triage process for mass casualty situations, supply room management, patient privacy issues and electronic medical records.
They see first-hand the roles of everyone on the medical team, such as medics, nurses and pharmacists. The concept of physician assistants was particularly new to them, said Dr. McDaniel. He explained that most physicians in Iraq have to handle patient care alone, but that encourages them to take a more thorough approach to physical exams.
“U.S. physicians are quicker to stop and order tests,” he said, adding that this is at least in part because testing facilities are not always available in Iraq, and the physician is often the only clinician in a large area. “[Iraqi physicians] have learned to do everything for themselves.”
At the end of each two-week session, the participants give a 15-minute presentation on an interesting aspect of a clinical case that they saw, which Dr. McDaniel compared to presentations that might be given by an intern in the U.S. Then they have a small graduation ceremony and receive certificates of completion.
“Having those certificates can really help them with their careers,” Dr. McDaniel said. “They truly appreciate the opportunity we are giving them.”
Making their mark
Both doctors used their own unique expertise to help enhance the program.
Dr. Slim, who is of Lebanese descent and lived in Lebanon with his family until he was 19, found that being from a similar culture helped him better adapt the training to the Iraqi doctors' needs.
“It made me able to understand their challenges and mission, but the Army provides all providers with frequent multi-cultural training prior to deployment that makes their mission easier,” he explained.
Preventive care is often lacking in Iraqi medicine, and as a cardiologist, Dr. Slim was able to teach the participants how to take a comprehensive approach to managing patients with heart disease by encouraging changes in exercise, diet and smoking habits.
Similarly, both doctors used their personal strengths to help participants maximize what they got out of the program.
Dr. McDaniel said he frequently suggested resources that the participants could use later, such as online training modules and websites with useful clinical practice guidelines.
Dr. Slim began assessments of participants' clinical and operational knowledge with questionnaires and also asked them where they believed their knowledge and health care resources were deficient. Based on their answers, he developed specialized seminars and clinical procedure training.
He repeated the assessments at the end of the program and found their “after” scores were dramatically higher than their “before” scores, from about 35% correct answers to 85%, he said.
He also started didactic lectures and created a website with links to American and European practice guidelines that participants can access at any time, even after they've completed the program. “Most of them do have computers with Web access,” he said.
Following up
Dr. Slim is working on a manuscript discussing the performance improvement in participants' knowledge and offering suggestions on what the Iraqi health care system needs.
“Being part of this program gave me great insight that I hope to share when I return [to the U.S.],” he said in an interview conducted while he was still in Baghdad.
At the top of that list is providing more access to evidence-based medicine.
“They do not have standardized guidelines for treatment as we do in the U.S. and most therapy is based on personal experience or outdated books due to lack of resources,” Dr. Slim explained.
Cultural differences also impact the providers' ability to fully apply the guidelines. Iraqi patients often feel as though they were not treated properly for an acute problem unless they receive some form of IV therapy, for complaints ranging from hypertension to headache.
“This makes the practice of evidence-based medicine very difficult to achieve until that piece of cultural misconception is resolved,” Dr. Slim said.
Learning goes both ways
Dr. McDaniel stressed that the learning in the program is not a one-way street.
“They learned a lot from us about our system of medicine, but they also took the time to teach us about Iraq's culture, history, customs and language,” he said. “It helped us all build better relationships.”
Dr. Slim agreed that the program benefits both sides, and stressed that its mission extends far beyond the teaching of technical skills.
“We provide care to everyone regardless of their nationality,” he said. “Seeing that happen forms a bridge that links our cultures.”