Why and how to monitor hypertension at home
Home measurement of high blood pressure overcomes variability inherent in office measurements, delivers better assessment of systolic pressure (and hence, of possible cardiovascular events) and offers a better chance of discontinuing drug therapy.
While some hypertension control initiatives bring patients into the office more often (see “Group visits bring focus and control to hypertension “ in this issue), another promising means of lowering blood pressure may be right in patients' living rooms.
“Home blood pressure measurement is practical, feasible and gives you good measures of hypertension control and the risk of cardiovascular disease,” said Mahboob Rahman, ACP Member, a nephrologist and associate professor at Case Western Reserve University in Cleveland.
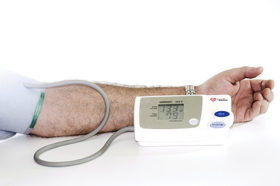
Dr. Rahman further described why, and how, physicians should use home-based blood pressure monitoring to attendees at the annual meeting of the American Society of Nephrology, held in Denver in November.
Office-based blood pressure measurement has multiple limitations as a method of monitoring hypertension control, Dr. Rahman said.
“Part of the problem is there is inherent variability in blood pressure and when we measure blood pressure once every few months or once every month, we simply aren't fully estimating the burden of hypertension in our patients,” he said. This limited picture is even more of a problem in treating patients who have masked or white coat hypertension.
Obviously, home measurement can correct both issues. It also offers additional advantages. “Home blood pressure actually predicts the risk of cardiovascular events better than conventional measuring,” said Dr. Rahman.
He described the results of a Finnish study, published in Hypertension last June, which found that systolic pressure measured at home was a significant predictor of cardiovascular events while office-measured was not. “Particularly at blood pressure over 135 or 140, home blood pressure is becoming a more sensitive measure of cardiovascular risk than is office-based blood pressure,” said Dr. Rahman. “There have been several studies in the past that have shown this.”
Research has also indicated that patients who measure blood pressure at home may adhere to their medication regimens more consistently. A 2006 meta-analysis, published in Clinical Hypertension, found several studies that reported a significant improvement in adherence associated with home monitoring, but also a few that didn't.
Other studies have indicated that home monitoring had a beneficial effect on the need for antihypertension medication.
“What they showed was patients who were assigned to the home monitoring were more likely to be able to come off of their drug therapy. Patients assigned to home monitoring were less likely to proceed to multiple drug treatment,” said Dr. Rahman. Home monitoring has also been shown to be an effective tool in management of antihypertensives for dialysis patients.
In light of the research, experts in many parts of the world have recommended home monitoring. “Most of the guidelines tell us that measurement of blood pressure at home should be a part of our assessment of hypertension patients,” Dr. Rahman said.
The guidelines also offer some specifics on how to use the information gathered from home monitoring. “At home, a blood pressure of greater than 135/85 is what you would consider elevated. This a little bit lower than the traditional 140/90,” he said.
Another issue is what kind of monitor to use. “Most of us would recommend a validated automated arm monitor that has memory,” said Dr. Rahman. “Some patients will ask you about using wrist monitors, finger monitors. The guidelines are fairly consistent that at least at this point in time, wrist and finger monitoring is not recommended.”
The monitor should also be one that has been validated. Dr. Rahman recommended a nonprofit website for information about different blood pressure monitors. In addition to educating patients about monitors, physicians should also mention some of the usual caveats: Get an appropriate-sized cuff, don't use tobacco or caffeine for 30 minutes before measuring, measure after five minutes of rest, use the nondominant arm or the one with the highest pressure, and keep the arm at heart level with the back supported and feet flat on the ground.
Typically, home measurement is done for a seven-day period. Patients measure their pressure two or three times every morning and two or three times in the evening. The first day's results should be excluded as patients get used to doing the measurements. The whole process should be repeated once per quarter of the year, Dr. Rahman advised.
Every once in a while, physicians should also have patients bring their monitor to an office appointment. “It's a good habit to check the blood pressure monitor readings periodically against a validated instrument at your office,” he said.
Once the home monitoring data are collected, the next issue is what to do with them. Dr. Rahman recommended an algorithm published in the Journal of the American Society of Hypertension in March/April 2010. The algorithm calls for home monitoring in patients with target organ disease or diabetes who have a pressure of over 130/80 and other patients at 140/90. If the home measurement results are under 125/75, nondrug therapy should be used and the monitoring repeated in three months. If the home measurements are over 135/85, antihypertensive drugs should be considered.
Patients with readings between those two cutoffs should receive ambulatory monitoring, according to the algorithm. Ambulatory monitoring has advantages of capturing short-term variability and readings during sleep, but it's more expensive and less convenient for patients than home monitoring, Dr. Rahman noted. “I think these are technologies that complement each other,” he said.
Future research will more definitively determine the best uses for both of these technologies, according to Dr. Rahman. “Studies are ongoing that should help us really look at hard outcomes,” he said.





