The timing is right, and possibly expandable, for giving tPA
Tissue plasminogen activator (tPA) was the star of the show at this year's International Stroke Conference 2009, with much discussion of expanding its treatment window, and several studies presented on gender differences in tPA treatment.
SAN DIEGO—Tissue plasminogen activator (tPA) was the star of the show at this year's International Stroke Conference 2009, with much discussion of expanding its treatment window, and several studies presented on gender differences in tPA treatment. The conference was sponsored by the American Heart Association/American Stroke Association.
tPA: Timing is everything
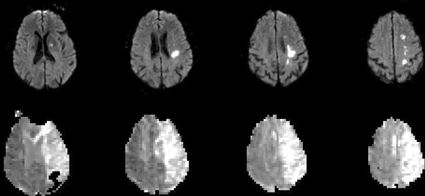
As expected, the timing of tPA administration was a top issue for speakers, researchers and other conference attendees, given the recent publication of a study saying it may be safe to expand beyond three hours the time for treating patients after stroke symptoms start. The European Cooperative Acute Stroke Study (ECASS III), published in the September 25 New England Journal of Medicine, found that acute ischemic stroke patients treated with tPA at 4.5 hours fared better than those taking placebo, and the patients didn't have higher rates of symptomatic intracerebral hemorrhage or death than patients who got tPA within three hours.
There are still questions about the ECASS III study, however, since the imaging used was “far from state of the art,” and there were many exclusions in the patient selection process, said Marc Fisher, MD, a neurology professor at the University of Massachusetts Medical School, who spoke about acute stroke treatment after three hours.
“The bottom line question is, ‘How generalizable are the results?’” Dr. Fisher said, adding that it is plausible to extend the tPA window to 4.5 hours for patients who meet the same criteria for enrollment as those in ECASS III, but not for others. “We need more trials on later time windows.”
New research presented at the conference supported the notion that, whether or not the time window is expanded, early arrival to the hospital is always preferable. The study found that patients who arrive at hospitals within an hour of stroke symptom onset are more than twice as likely to get tPA as those who arrive in the second or third hour. Specifically, the registry study of more than 100,000 patients found that 27% of those who arrived within an hour of symptom onset got tPA, compared with 13% who arrived between one and three hours after onset.
“Prior studies have suggested that 25% to 30% of early arriving patients are fully eligible,” for tPA, thus the hospitals in the study were giving treatment to virtually all eligible patients, said Jeffrey Saver, MD, the study's lead author and director of the Stroke Center at the University of California, Los Angeles.
The bad news, however, was that physicians took nearly 15 minutes longer to treat first-hour patients than those who arrived later, perhaps thinking they had more time to ensure that treatment was the right decision, Dr. Saver said. Current guidelines recommend a “door-to-needle” time for tPA of 60 minutes from hospital arrival; for the study patients, the door-to-needle time was 90 minutes.
“There are a huge number of reasons for waiting (to give treatment), but they are all trumped by the fact that the longer you wait, the more the brain dies,” Dr. Saver said.
The study also revealed that 28% of ischemic stroke patients arrive within 60 minutes of symptom onset, 31.7% arrive between one and three hours after onset, and 40% arrive more than three hours after symptoms start. Patients who arrived in the first hour had significantly more stroke deficits than those who arrived later, suggesting their more intense symptoms encouraged them to get medical help earlier, Dr. Saver said.
Gender differences
Several new studies examined differences between men and women in terms of receiving treatment, and in long-term outcomes after stroke. Two looked at whether men and women are treated differently with tPA for acute stroke. The first, a meta-analysis of 18 studies and 2.3 million acute stroke patients, found that women's overall odds of getting tPA were 30% lower than men's—a significant difference. However, a sub-group analysis of four studies, in which all patients had arrived at the hospital within the official three-hour window for getting tPA, found that women were 19% less likely to get treatment—no longer a statistically significant difference. The article was published in the February Stroke.
The second, a retrospective study of 445 patients, found that women arrived at the emergency department (ED) of a tertiary stroke center later than men, but were treated just as quickly and often as men once they got there. This suggests that women may get tPA treatment later because they arrive later to the ED, when physicians may be more reluctant to use tPA for fear of missing the treatment window, said study co-author Louise McCullough, MD, director of stroke research and education at the University of Connecticut Health Center in Farmington, Conn.
“Why are women losing time getting [to the ED]? Maybe because women are older when they are having strokes, or they outlived their husbands and there is no one to tell or call [when symptoms start], or they aren't identifying symptoms,” Dr. McCullough said. “Educational campaigns need to target women and focus on identification of warning signs, and on the importance of immediate medical evaluation.”
Another study found that elderly women are less likely than elderly men to be readmitted to the hospital for stroke or heart disease, or to die, in the month or year after having a transient ischemic attack (TIA). TIA can be an important signal of more serious problems, as nearly one in six people who have a TIA will have a stroke within six months.
Using Medicare administrative records of 122,063 hospital discharges for TIA, with a mean patient age of 79 years, researchers found women were 15% less likely than men to be readmitted for stroke, 19% less likely to be readmitted for heart disease, and 12% less likely to die, one year after having a TIA. The study was published in the February Stroke.
In explaining the results, study co-author Judith Lichtman, PhD, associate professor at Yale University School of Medicine, said it may have to do with differences in the underlying stroke etiology between men and women.
“Large artery atherosclerosis, which is associated with a higher stroke risk, may be more likely to be the cause of TIA in men,” Dr. Lichtman said. “There doesn't seem to be a difference between men and women in recognition of TIA, or in treatment. In fact, women are often treated less aggressively than men.”
In a session on stroke outcomes in men and women, speaker Michael Hill, MD, associate professor in the department of clinical neurosciences at the University of Calgary, Alberta, Canada, said several studies have shown women fare worse than men if they don't get tPA when they should. On the other hand, women do about the same as men when they are treated with tPA.
“We don't know yet why this is true. It could be because women have smaller arteries, or because of metabolic syndrome effect differences between men and women, or it could be because women live longer and have no caregiver, so their long-term outcomes after discharge are poorer,” Dr. Hill said.
It's important that future research tease out the reasons behind these gender differences, since women account for 61% of stroke deaths, and stroke is expected to become more prevalent in future years as the population ages, noted speaker Helmi Lutsep, MD, of the Oregon Stroke Center at Oregon Health and Science University in Portland, Ore.





