MKSAP Quiz: Worsening thrombocytopenia
A 35-year-old woman is evaluated for worsening thrombocytopenia; she is pregnant at 36 weeks' gestation. Medical history is significant for immune thrombocytopenic purpura. Previous platelet counts during this pregnancy have been 80,000 to 100,000/µL (80-100 × 109/L). Her only medication is a prenatal vitamin.
On physical examination, temperature is 37.0°C (98.6°F), blood pressure is 165/110 mm Hg, pulse rate is 95/min, and respiration rate is 18/min. Abdominal examination reveals mild right upper quadrant discomfort on palpation. Reflexes are normal, and no clonus is observed. She has lower extremity edema to the level of the knees bilaterally.
Laboratory studies:
| Hemoglobin | 10.5 g/dL (105 g/L) |
| Platelet count | 21,000/µL (21 × 109/L) |
| Alanine aminotransferase | 480 U/L |
| Aspartate aminotransferase | 600 U/L |
| Creatinine | 1.2 mg/dL (106.1 µmol/L) |
| Urinalysis | 3+ protein |
A peripheral blood smear is shown.
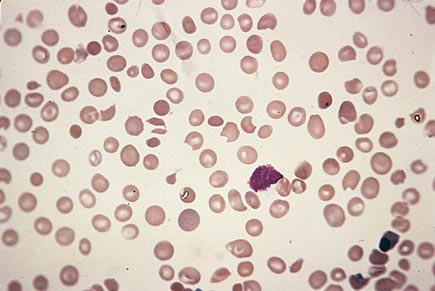
Which of the following is the most appropriate management of this patient's thrombocytopenia?
A. Emergent delivery
B. Intravenous immune globulin
C. Plasma exchange
D. Prednisone
Answer and critique
The correct answer is A: Emergent delivery. This question can be found in MKSAP 17 in the Hematology & Oncology section, item 8.
The most appropriate management for this patient's thrombocytopenia is immediate delivery of the fetus, because she has HELLP (Hemolysis, Elevated Liver enzymes, and Low Platelets) syndrome. Although she has a history of immune thrombocytopenic purpura (ITP), and her platelet counts have been low throughout the pregnancy, her markedly decreased platelet count is worrisome and could indicate development of another condition. Worsening anemia, right upper quadrant pain, hypertension, proteinuria, and elevated liver enzymes are more consistent with a microangiopathy of pregnancy (HELLP syndrome, pre-eclampsia, thrombotic thrombocytopenic purpura [TTP]) rather than worsening ITP. Her clinical picture is more consistent with preeclampsia (new-onset hypertension at >20 weeks' gestation) with proteinuria or the HELLP syndrome. The relationship between pre-eclampsia and HELLP syndrome is unclear; HELLP syndrome occurs in 10% to 20% of women with preeclampsia but occasionally in some patients without hypertension or proteinuria. The primary treatment for both conditions, particularly in advanced pregnancy, is urgent delivery. Platelet counts tend to recover quickly after delivery; persistent thrombocytopenia several days after delivery should raise concern for another diagnosis, such as thrombotic thrombocytopenic purpura–hemolytic uremic syndrome (TTP-HUS).
Administering intravenous immune globulin is not indicated as a treatment for thrombocytopenia associated with pre-eclampsia and HELLP syndrome.
Plasma exchange can be undertaken if TTP is present earlier in the pregnancy before delivery is a viable option, but would not be a preferred treatment strategy in a patient in whom delivery is appropriate. Plasma exchange would be indicated if thrombocytopenia persisted after delivery and TTP-HUS were diagnosed.
Glucocorticoids such as prednisone are not indicated for microangiopathy of pregnancy. Additionally, if used as a treatment for ITP, prednisone typically takes 48 to 72 hours for effectiveness. Therefore, treatment with prednisone would not be appropriate in this patient.
Key Point
- Immediate delivery of the fetus is the best management approach for pregnant women experiencing thrombotic microangiopathy of pregnancy.




