Intertwining patients in their care management
Patient autonomy is the key to an app that puts patients in control of meeting their goals to reduce high blood pressure.
The issue: Engaging patients in management of their hypertension.
Background
As a medical resident, John O. Moore, MD, PhD, was frustrated by the lack of opportunity to help his patients manage their chronic diseases between office visits.
“We're still treating them as if we just need to figure out the diagnosis and tell them the treatment, and that's magically going to fix things,” he said. “But people don't want to simply be told what to do. That is why there is such a disconnect between medical recommendations and actual behavior when it comes to chronic diseases. What people need is a way to be involved in creating the plans for their care ... and they need tools that help [them] to learn and self-reflect and experiment and see for themselves the benefits and the drawbacks of different approaches.”
After he left medical practice to be a researcher at the Massachusetts Institute of Technology Media Lab in Cambridge, Mass., he tried to develop such a tool. “We explored everything from games to intelligent avatars to automated systems that really just tell you what you need to do and you do it,” said Dr. Moore. However, patient autonomy turned out to be a critical component of the solution he and his colleagues eventually developed.
How it works
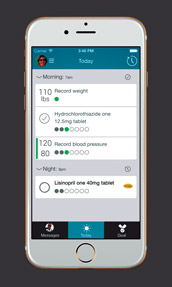
Their tool, called Twine, is a cloud-based software platform with apps for both patients and clinicians that allow them to set goals for the patients' care and then monitor their progress toward those goals. For example, in a trial of the concept, patients with uncontrolled hypertension used wireless home blood pressure monitors to track and report their blood pressures. They also reported their medication adherence using a tablet loaded with the tool.
Another important component is back-and-forth instant communication between the patient and a coach. “Sometimes that coach is a nurse, either an RN or an LPN. Sometimes that person is not clinically trained, but the common component is that the coach is there to provide timely support in the face of challenges and praise when success is achieved,” said Dr. Moore, who is now CEO of Twine Health.
Coaches are notified by the system when a patient sends a message or if a patient's goals are not being met. “It shows who's struggling with adherence to their plan, or who is adherent to their plan but their plan isn't achieving the desired outcome. That way the coach doesn't have to look at every blood pressure, every blood glucose, or every medication adherence. Instead they see, ‘Who needs my help today?’” said Dr. Moore.
Coaches frequently contact patients with assistance to get to their goals, but after the initial goal-setting, physicians are only involved if a change in medication regimen is needed.
Results
In the initial 42-patient trial, significantly more patients who used the system lowered their systolic blood pressure compared to controls. Fifteen patients in the intervention group achieved a blood pressure of 130/80 mm Hg or better, compared to only 7 of the controls, according to results published in the March 2014 Journal of Clinical Outcomes Management.
As the tool has expanded into health systems scattered around the country, the results have continued to be positive. “We currently have 278 patients using Twine, and 92% currently reach goal blood pressure within 3 months,” said Dr. Moore. Twine also tracks its own efficiency, recently posting statistics like 12 minutes of coach time per patient per month. “Quite easily, [a coach using Twine] can care for 500 patients, which is 5 times more than a typical care coordinator in a medical system,” he said.
Patients also give the system positive reviews, even those who might not be expected to adopt new technology. “We found that it doesn't matter—young, old, rich, poor, techie, non-techie,” said Dr. Moore. “We've worked with patients in their 90s. Many of those patients had never used a smartphone or a tablet before in their life. Some of them had never even used a computer before, but they learned Twine in no time.”
The key factor in whether the system works for a patient is whether he or she has felt disempowered in his or her health care and would like a more active role, according to Dr. Moore. “The reason that patients really perceive it as a really positive experience is because that patient helped create that plan for themselves,” he said.
Challenges
As with so many innovations, the biggest challenge is how to pay for the tool under a fee-for-service system. “We don't have any problem getting people interested in using this,” said Dr. Moore. “How do we scale up when the [health care system's] economics are in such flux?” The continuing shift to value-based payment should help, as well as growing evidence of Twine's cost-effectiveness, he added.
Next steps
In addition to hypertension treatment, the tool now supports weight loss efforts and diabetes care. Next up are depression, congestive heart failure, chronic obstructive pulmonary disease, and asthma. Dr. Moore eventually envisions the tool as a component in many patients' ongoing health care.
“Maybe for the next 3 months, you have a goal for your diabetes, but maybe another month from then, you're pregnant and doing your prenatal care through Twine ... Maybe I've reached my blood pressure goal and now I want to get off of one of my medications. Or maybe now, I want to address my depression,” said Dr. Moore. “What we hope is to create a relationship between patient and Twine where they always are working on new goals.”
Words of wisdom
Dr. Moore hopes physicians and practices will join him in this effort. “Anyone who wants to adopt Twine, it's ready,” he said. “There's this conception that to adopt a new tool like this takes tons of money and tons of time and lots of red tape.” In fact, however, practices have launched the tool in as little as 3 days and Twine costs $4 per patient per month, Dr. Moore said. He predicts that the time required for launch will soon be down to a few hours.