Sussing out sleep apnea disorders
Given the prevalence of poor sleep habits, determining sleep apnea can be difficult during a time-pressed visit. Asking the rights questions is key.
Given the number of patients who report fatigue, sorting out self-inflicted poor sleep habits from sleep apnea is far from a slam dunk during a time-pressed office visit.
Yet primary care doctors remain on the front lines of detecting the common condition, which has potentially long-term medical effects, said James Rowley, MD, ACP Member, a pulmonologist and sleep medicine specialist at Wayne State University in Detroit. “I think the challenge,” he said, “is taking the time to ask the right questions.
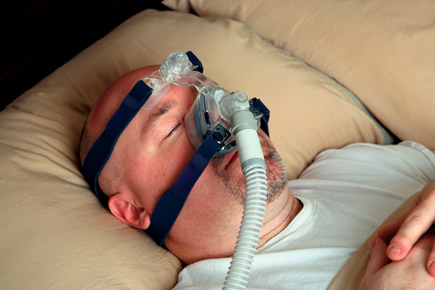
Sleep apnea is estimated to impact as many as 17% of Americans, according to data cited in recently published diagnostic guidelines from the American College of Physicians. It's been associated with a variety of other conditions, including hypertension, heart disease, and cognitive effects.
The guidelines, published last August in Annals of Internal Medicine, outline the various strengths and weaknesses of sleep studies and questionnaires in sorting out a diagnosis. At this point, diagnostic efforts should focus on patients who report perplexing daytime sleepiness, the authors concluded, as research shows that it's the symptom most responsive to treatment.
Several months after the Annals guidelines appeared, the National Transportation Safety Board also spotlighted the safety implications of undiagnosed apnea. In its report investigating a series of train accidents in the Northeast, the federal agency issued a series of recommendations. Among them, they asked officials at both ACP and the American Academy of Family Physicians to “enhance initial and ongoing training” to ensure that patients with sleep apnea are identified and treated.
Dr. Rowley supports the agency's efforts to boost sleep awareness. Ideally, every patient should be asked about sleeping patterns during an annual physical, he said. Do they snore? Do they awake refreshed? Do they take naps during the day or feel sleepy at work?
At minimum, doctors should pursue such questions if a patient's body mass index reaches 30 or higher, he said. Plus, any patient with a transportation-related job should be monitored for sleep apnea, as should factory workers who operate heavy machinery—really, he said, “anyone in a job that has potential risks to the public.”
Flagging apnea
Sleep frustrations remain a pervasive problem, with 35% of Americans reporting that their quality of sleep is “poor” or “only fair,” according to a National Sleep Foundation poll conducted last year involving 1,250 people. But the number of Americans suffering from sleep deprivation related to sleep apnea has been difficult to nail down. The ACP guidelines cite prevalence estimates ranging from 10% to 17%. In the sleep foundation's poll, nearly 12% said that they had been diagnosed.
Apnea, which translates as “without breath” in Greek, breaks down into 3 types: obstructive, central, and mixed. The ACP guidelines focus on obstructive sleep apnea, the most common form. It develops when the airway collapses or becomes blocked in some way during sleep, causing more shallow breathing or gaps and related sleep disturbances. In central sleep apnea, the brain is involved, failing to signal the muscles to breathe. Mixed apnea is a combination of the two.
While a causal connection has yet to be shown, obstructive sleep apnea is associated with a number of worrisome conditions, including heart disease, hypertension, and cognitive effects, according to the guidelines. The strongest evidence shows a link between an apnea-hypopnea index of greater than 30 events per hour and higher mortality overall, the authors wrote. For those with the most severe sleep apnea, the overall mortality rate can be 3 times higher than in those without the condition, according to a 2008 study, published in the journal Sleep, which analyzed 18 years of mortality data from a group of Wisconsin patients.
But some conditions are more closely associated with sleep apnea or could potentially be relieved at least in part by treating the disorder, Dr. Rowley said. Patients with heart failure are more likely to have either obstructive or central apnea and thus should be regularly screened, he said. There also is some evidence that patients with persistent hypertension despite taking multiple medications might be helped if their sleep apnea was caught and treated, he said.
Another intriguing area of research is looking at whether apnea might be associated with glucose control, said Andrew Varga, MD, PhD, a neurologist and attending physician in the Sleep Disorders Center at New York University Langone Medical Center. But it's difficult to sort out the chicken-and-egg conundrum, he pointed out. For example, diabetes already is associated with obesity, and obesity is a risk factor for sleep apnea.
Other research is delving into potential effects on thinking. Dr. Varga recently coauthored a study, published online Oct. 29, 2014, in the Journal of Neuroscience, finding that deficits in the REM sleep of those with obstructive sleep apnea appear to undercut their spatial memory skills. When Dr. Varga evaluated the skills of 18 participants with severe sleep apnea by tracking their performance on a maze-like video game, he found that they were more effective when sleep was consolidated by using continuous positive airway pressure (CPAP) than when their REM sleep had been interrupted by apnea in the sleep lab.
Sometimes, the symptoms of apnea can emerge somewhat gradually, perhaps over many years, so there's not necessarily a notable shift in sleeping patterns that the patient will bring up, said David Claman, MD, medical director of the UCSF Sleep Disorders Center in San Francisco. If a patient comes in during a routine appointment and says he is snoring too much and his spouse wants something done about it, that can provide the doctor the opportunity to ask related questions, such as if there have been any nighttime gaps in breathing, he said.
Otherwise, he added, “For a lot of internists, asking about sleep has traditionally not been one of the basic parts of assessing a patient.”
Questionnaires and beyond
In its evidence review, the ACP guidelines compiled research involving 5 different screening questionnaires and found little evidence that they could be helpful. They “may not be all that accurate,” said Paul Dallas, MD, FACP, a coauthor on the guidelines and an assistant professor in the department of medicine at Virginia Tech Carilion School of Medicine in Roanoke, Va.
The problem is that the quality of the evidence is low and there's too wide a range in sensitivity and specificity to be of much diagnostic value, Dr. Dallas said. But the questionnaires, such as the Berlin or the STOP-BANG, might serve as a tool to get the internist thinking more about the condition, Dr. Claman said. Since a questionnaire typically takes just a handful of minutes to fill out, Dr. Rowley suggested adding it to the queries about alcohol consumption and other screening paperwork that the patient completes in the waiting room.
Among its 2 primary recommendations, the diagnostic guidelines focused on sleep studies, recommending a study for any patient with unexplained daytime sleepiness. They also recommended that patients with suspected obstructive sleep apnea be referred for polysomnography. Portable sleep monitors might be an option in those individuals without other serious medical conditions, such as congestive heart failure, when polysomnography is not available, the guideline authors wrote.
The evidence review didn't find any head-to-head studies involving the portable home-based monitor options, Type II through Type IV, Dr. Dallas said. But when their accuracy is assessed compared with polysomnography, Type II monitors appear better for diagnosis than the other two, he said.
Both polysomnography and the Type II monitor can measure the apnea-hypopnea index, showing the number of such events, Dr. Dallas said. To be diagnosed with obstructive sleep apnea, a patient without symptoms must exhibit at least 15 events per hour and a person with symptoms must exhibit at least 5 events per hour, according to the American Academy of Sleep Medicine. The academy lists numerous potential symptoms, including daytime sleepiness, unrefreshing sleep, fatigue, and waking up gasping, as well as someone else witnessing loud snoring or breathing interruptions. Those apnea-hypopnea index scores also are used by Medicare officials when they determine whether to reimburse for treatment with CPAP devices.
But Type III and Type IV monitors can't tell whether an individual is awake or asleep, and therefore they only provide estimates rather than directly measuring apnea-hypopnea index episodes, Dr. Dallas said. The guidelines also note that Type IV monitors can't differentiate between obstructive and central sleep apnea.
One area where primary care doctors can play a significant role is emphasizing to their patients the potential medical risks they face if they don't get help, said Kristen Knutson, PhD, a faculty member in the Sleep, Metabolism and Health Center at the University of Chicago. Data show, she said, that “patients are referred for a sleep study but don't go. And if they get the sleep study, they might not follow up for treatment.”
Breathing easier
If a patient declines a sleep study or is unwilling to try CPAP, there are some other steps they can attempt first, starting with losing weight, Dr. Claman said. Doctors also can educate patients about sleep strategies, such as avoiding alcohol close to bedtime and sleeping on their sides instead of their backs, he said. “Occasionally we do see people who take those seriously and successfully and don't need the CPAP.”
CPAP is recommended as the initial line of treatment once a patient is diagnosed with obstructive sleep apnea, according to ACP's clinical guidelines on management, also published last year in Annals of Internal Medicine. Those guidelines recommended mandibular advancement devices as an alternative for those patients who prefer that approach or have difficulties with CPAP.
CPAP devices have become smaller and quieter, along with other adjustments designed to keep them in place and make them more comfortable, Dr. Claman said. But convincing patients to wear them nightly for the recommended 5 to 6 hours remains challenging, he said.
Primary care doctors can check whether patients are still using the device during office visits for any other reason, Dr. Rowley said. If they have set the device aside, the doctor can refer them back to the sleep specialist and provide reassurance that steps can be taken to improve comfort.
In some cases, a switch to another style of mask can make the difference, Dr. Rowley said. Sometimes the devices are causing nasal congestion or a dry mouth, and medications can be prescribed to relieve that.
“I will tell you that patients who love it, love it,” he said. “It's just really a matter of helping a patient get to the point that maybe they don't love it, but they are going to use it to the point that they feel better.”
It's understandable that busy primary care doctors are so focused on treating the immediate medical issue at hand that sleep difficulties never cross their mind, said Dr. Dallas, a general internist. But a bit more awareness can provide some unexpected relief to patients who didn't even realize why they were suffering, he said.
Consider the male patient who arrives at the exam room complaining of knee pain. He's also packing 220 pounds on his 5-foot 6-inch frame, his neck is thick, and his blood pressure is creeping up. Perhaps this is a good opportunity to ask a few sleep-related questions, Dr. Dallas said. “With today's obesity epidemic, we ought to be thinking about it more and more.”