MKSAP Quiz: Abrupt onset of chest pain
A 67-year-old woman is evaluated for the abrupt onset of right-sided pleuritic chest pain and moderate dyspnea. She recently had symptoms typical of an upper respiratory infection (rhinorrhea, headache, sore throat and nonproductive cough), and her chest pain and dyspnea seemed to be triggered by an episode of vigorous coughing. She has not had fever, chills, purulent sputum, or risk factors for thromboembolic disease. She smokes, and her medical history is significant for COPD without additional complications. Her medications are daily salmeterol and as-needed albuterol.
On physical examination, she appears uncomfortable but is not in respiratory distress. She is speaking in full sentences. Temperature is 37.0°C (98.6°F), blood pressure is 129/58 mm Hg, pulse rate is 78/min and regular, and respiration rate is 22/min. Oxygen saturation is 98% on 2 L of oxygen via nasal cannula. Pulmonary examination is significant for a prolonged expiratory phase but no wheeze; breath sounds are symmetric bilaterally. The trachea is midline. There is no accessory muscle use. Cardiac examination is normal with no murmurs. No edema is noted.
Electrocardiogram shows normal sinus rhythm without ischemic changes. Chest radiograph is shown.
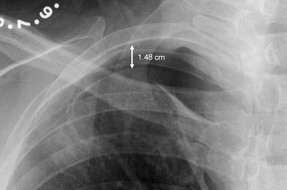
In addition to hospital admission, which of the following is the most appropriate next step in management?
A. Evaluation for pleurodesis
B. Needle aspiration
C. Serial chest radiography
D. Tube thoracostomy
Answer and critique
The correct answer is C: Serial chest radiography. This question can be found in MKSAP 16 in the Pulmonology and Critical Care section, item 8.
The most appropriate next step in management is serial chest radiography. This patient presents with a small, spontaneous pneumothorax in the setting of known COPD. The pneumothorax is therefore classified as a secondary spontaneous pneumothorax. In this case, there is less than 2 cm between the chest wall and lung, and it is reasonable to observe the pneumothorax with serial chest radiography rather than intervene at this time. Given the decreased respiratory reserve and higher likelihood of progression and mortality in this patient group when compared with patients without known underlying structural lung disease (primary spontaneous pneumothorax), observation should be performed in the inpatient setting.
If a persistent air leak is noted after 3 to 5 days, it is reasonable to consider definitive treatment of the pneumothorax. Definitive management to prevent recurrence typically consists of chemical pleurodesis via thoracostomy (which is shown to reduce recurrence to 25%) or thoracoscopic repair with pleurodesis (which reduces recurrence to approximately 5%).
Needle aspiration is an option for treating secondary pneumothoraces, but it has been shown to be significantly less effective than tube thoracostomy in patients requiring therapeutic intervention.
If at any time the pneumothorax increases to greater than 2 cm, a small-bore chest tube should be placed, because the patient is experiencing dyspnea.
Key Point
- For secondary spontaneous pneumothoraces, outpatient management is discouraged; even small (<2 cm) pneumothoraces are more safely observed in the inpatient setting.




