MKSAP Quiz: Several-month history of pruritic rash
A 20-year-old woman is evaluated for a several-month history of unintentional weight loss, diarrhea, poor glycemic control, and pruritic rash. She was diagnosed with type 1 diabetes mellitus 2 years ago. Medications are insulin glargine and insulin aspart injection.
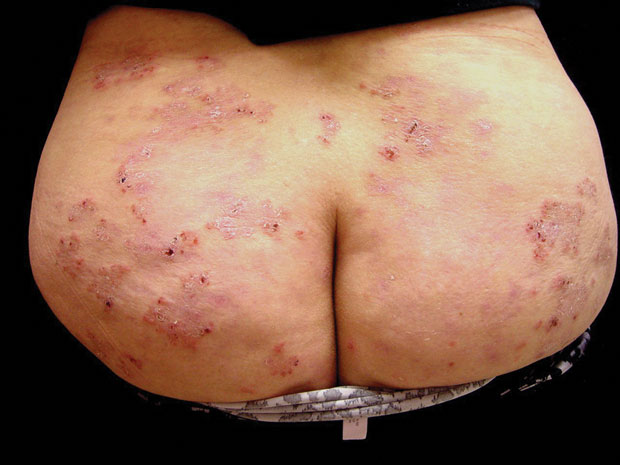
On physical examination, vital signs are normal. BMI is 20. A rash is symmetrically distributed over her knees, elbows, sacrum, and buttocks. A representative sample of the rash is shown. No abdominal tenderness is noted. The remainder of the examination is normal.
Which of the following is the most appropriate diagnostic test to perform next?
A. Colonoscopy
B. Gastric emptying study
C. IgA tissue transglutaminase antibody measurement
D. Thyroid peroxidase antibody measurement
Answer and critique
The correct answer is C. IgA tissue transglutaminase antibody measurement. This item is Question 8 in MKSAP 19's Endocrinology and Metabolism section.
This patient with type 1 diabetes mellitus and gastrointestinal manifestations or clinical signs of celiac disease should be evaluated for celiac disease with measurement of IgA tissue transglutaminase antibody (Option C). Patients with immune-mediated type 1 diabetes are at an increased risk for other autoimmune disorders, including celiac disease, thyroid disorders, vitiligo, pernicious anemia (autoimmune gastritis with intrinsic factor deficiency), autoimmune hepatitis, and autoimmune primary adrenal gland failure. Positive antibody tests should be followed by confirmatory duodenal biopsy. Consideration should be given to assessing total IgA level, and, if IgA deficiency is present, anti-deamidated gliadin peptide IgG antibodies or tissue transglutaminase IgG antibodies can be used. In the case of negative serologic tests with high level of suspicion, endoscopy with duodenal biopsy may be indicated. Classic celiac disease is an immune-mediated inflammatory disease involving the small intestine in response to sensitivity to dietary gluten. Celiac disease most commonly presents with diarrhea and evidence of malabsorption. A common skin manifestation is dermatitis herpetiformis, characterized by pruritic inflammatory papules and vesicles on the forearms, knees, lower back, sacrum, and buttocks. The vesicles rapidly break, leaving erosions.
Colonoscopy (Option A), although an important component of the evaluation of many patients with chronic diarrhea, is not indicated given the high likelihood of celiac disease. If the evaluation for celiac disease is negative, then colonoscopy would be a reasonable next test.
A gastric emptying study (Option B) would not be the most appropriate test. Although a complication of diabetes is gastroparesis, or delayed gastric emptying, it typically develops over a longer duration in a patient with poor glycemic control. Signs and symptoms include nausea, vomiting, early satiety, belching, bloating, or abdominal discomfort. Dermatitis herpetiformis is not associated with gastroparesis.
Classic signs and symptoms of Hashimoto disease, or autoimmune hypothyroidism, include fatigue, weight gain, bradycardia, constipation, cold intolerance, and dry skin. Patients with type 1 diabetes should be screened for primary hypothyroidism soon after diagnosis and periodically thereafter. The appropriate screening test is thyroid-stimulating hormone measurement (Option D). Thyroid peroxidase antibodies are present in most patients with Hashimoto thyroiditis, but measurement is usually unnecessary unless the diagnosis is unclear.
Key Points
- Patients with immune-mediated type 1 diabetes mellitus are at an increased risk for other autoimmune disorders, including celiac disease, thyroid disorders, vitiligo, pernicious anemia, autoimmune hepatitis, and autoimmune primary adrenal gland failure.
- Patients with type 1 diabetes mellitus and gastrointestinal manifestations or clinical signs of celiac disease should be evaluated with measurement of IgA tissue transglutaminase antibody.




