MKSAP Quiz: 2-week history of bloody diarrhea
A 24-year-old man is evaluated in the emergency department for a 2-week history of worsening bloody diarrhea with up to 10 bloody bowel movements per day. He also reports increasing lower abdominal pain and distension and that stool frequency has decreased over the past day. He has extensive ulcerative colitis of 5 years' duration. His medications are infliximab and azathioprine.
On physical examination, the patient appears ill. Temperature is 38.3°C (101°F), blood pressure is 90/60 mm Hg, and pulse rate is 110/min; other vital signs are normal. The abdomen is distended with guarding. Bowel sounds are hypoactive.
Laboratory studies show a hemoglobin level of 10 g/dL (100 g/L), leukocyte count of 16,000/µL (16 × 109/L), and blood urea nitrogen level of 26 mg/dL (9.3 mmol/L).
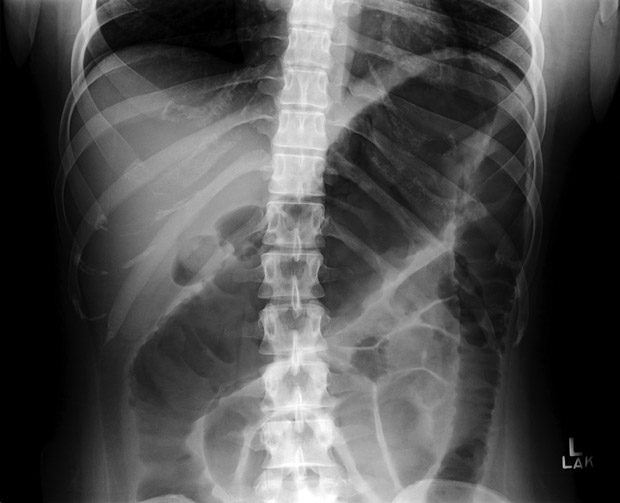
An abdominal radiograph is shown.
Which of the following is the most appropriate next step in management?
A: Colectomy
B: Colonoscopy
C: CT of the abdomen
D: Stool culture
Answer and critique
The most likely diagnosis is A. Colectomy. This question can be found in MKSAP 18 in the Gastroenterology and Hepatology section, item 14.
This patient requires colectomy. He has a history of ulcerative colitis and presents with fever, tachycardia, hypotension, and a dilated colon on abdominal radiography; the diagnosis is toxic megacolon, a life-threatening condition that complicates approximately 5% of acute, severe cases of ulcerative colitis. Toxic megacolon is defined by the presence of toxicity (fever, tachycardia, hypotension, and leukocytosis) along with evidence of colonic dilation. Patients with this condition have an increased risk for complications such as colonic perforation. Intravenous fluid resuscitation, intravenous high-dose corticosteroids, and broad-spectrum antibiotics (for example, a third-generation cephalosporin with metronidazole) should be initiated in patients with toxic megacolon. Management requires close collaboration with a surgeon; therefore, emergent surgical consultation for consideration of subtotal colectomy is required because of the impending risk for perforation and peritonitis in patients with toxic megacolon. Some patients may respond to medical therapy with high-dose glucocorticoids (in addition to intravenous fluids and broad-spectrum antibiotics), but there should be a low threshold for surgical intervention due to the potential harms associated with toxic megacolon.
Colonoscopy is contraindicated because it would increase the risk for perforation and complications related to toxic megacolon.
CT of the abdomen and pelvis is the optimal imaging modality to evaluate suspected toxic megacolon and may better assess for the presence of colonic necrosis; however, in this case, the diagnosis of toxic megacolon can be confidently made based on the patient's presentation and abdominal radiography, and urgent surgical evaluation is necessary.
Stool studies for enteric pathogens may identify a precipitant of toxic megacolon but require a minimum of 24 hours before test results are received. Surgical consultation should not be delayed to wait for results of stool testing.
Key Point
- Toxic megacolon is defined by the presence of toxicity and evidence of colonic dilation; it requires prompt surgical treatment.