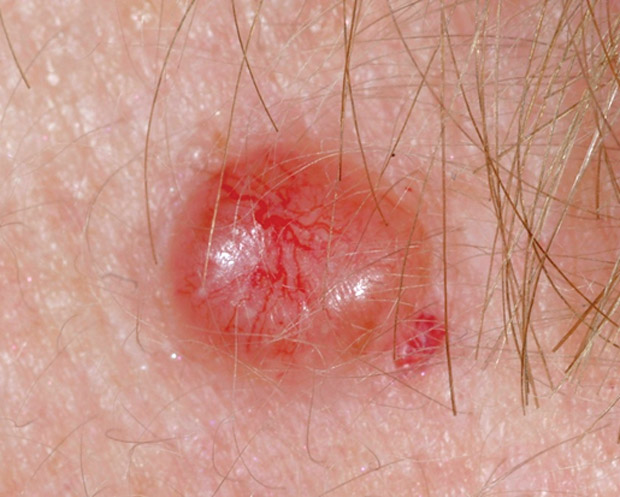
High-risk PCOS could benefit from internist management
This issue also covers transitional care, patient transportation, and a novel medical school course.
Polycystic ovary syndrome (PCOS) can be a challenge for both patients and physicians, given its bothersome symptoms, varying diagnostic criteria, and confusing name. In many cases, it may take years for the condition to be recognized and appropriately treated. Our story in this issue offers a rundown of the subtypes of the disease (including what one expert calls “internist PCOS”), the signs and symptoms internists should look for, the appropriate diagnostics tests to run, and the referrals that may be most appropriate.
Determining the best way to support high-risk patients, especially during times of transition, can be a daunting prospect. CMS now offers payment for transitional care management, defined as follow-up care by telephone calls or nonoffice visits within 30 days of a hospital discharge, but some believe the incentive is outweighed by the work involved to claim it. And while some patients may benefit greatly from more focused care, others may not benefit at all. Our story looks at some tools and programs that have been proven to help, as well as tips on how to determine what might work in your practice.
Continuing this theme, a story in this issue looks at the pros and cons of providing rides to patients to help them get to their medical appointments. Patients who are no-shows often give transportation as the reason, so offering subsidized rides through a taxi service or a ride-sharing company may seem like a no-brainer. But as with many initiatives, the reality is more complicated in practice. For example, maintaining a ride-sharing system can eat up a lot of staff time, and patients who are offered rides may end up missing their appointments for other reasons anyway. Learn more about programs that have tried ride-sharing, as well as an ambitious new pilot that is offering rides not just for doctors' appointments but for other medical reasons, such as picking up a prescription.
Medical students have a lot to learn in their standard curriculum, but an elective course recently developed at the University of Pennsylvania zeros in on observational skills by way of the fine arts. First-year medical students who choose this elective spend time studying and learning to describe the details of paintings and other artwork in order to help improve their descriptive abilities, as well as empathy and perspective.
Have you offered rides to patients in your practice? What's your opinion of art class in medical school? Let us know.
Sincerely,
Jennifer Kearney-Strouse
Executive Editor