MKSAP Quiz: New rash on legs
A 32-year-old woman is evaluated for a new rash on her legs. She was diagnosed with pyelonephritis 4 days ago and was started on a 7-day regimen of trimethoprim-sulfamethoxazole based on urine culture and sensitivity data; her urinary symptoms have improved. Medical history includes Hashimoto thyroiditis treated with levothyroxine; her dose was increased 4 weeks ago based on thyroid function studies. Medical history is otherwise unremarkable.
On physical examination, temperature is normal, blood pressure is 124/82 mm Hg, pulse rate is 66/min, and respiration rate is 13/min. BMI is 21. Cardiopulmonary examination is unremarkable. The abdomen is soft and nontender. Musculoskeletal examination shows no evidence of joint swelling, warmth, or tenderness. The remainder of the examination is normal.
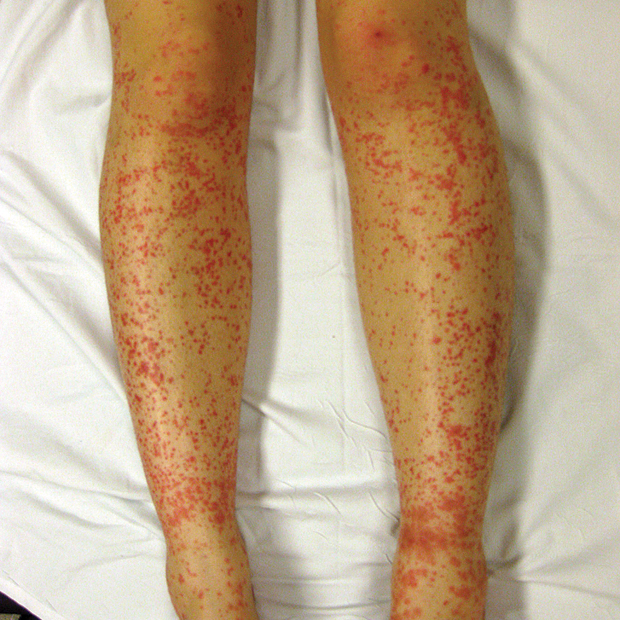
The appearance of the legs is shown.
Which of the following is the most appropriate next step in management?
A. Discontinue trimethoprim-sulfamethoxazole
B. Initiate prednisone
C. Measure antihistone antibodies
D. Obtain skin biopsy
Answer and critique
The most likely diagnosis is A. Discontinue trimethoprim-sulfamethoxazole. This question can be found in MKSAP 17 in the Rheumatology section, item 40.
Discontinuation of trimethoprim-sulfamethoxazole is indicated for this patient who developed palpable purpura within days of starting trimethoprim-sulfamethoxazole for a urinary tract infection. The most likely diagnosis is hypersensitivity vasculitis, which is caused by a hypersensitivity reaction to antigens such as medication or infection. Hypersensitivity vasculitis typically resolves when the offending agent is removed. Similar to other forms of small-vessel vasculitis, hypersensitivity vasculitis results from antibodies directed toward the antigens that result in immune complex formation. Complement is activated, and neutrophils are attracted to accumulate in capillaries, arterioles, and post-capillary venules. Although a similar reaction associated with the infection itself may occur, this is less likely given the time course of onset and the high degree of association of trimethoprim-sulfamethoxazole with this reaction. Because her reaction is mild and limited to the skin, the most important aspect of treatment is to remove the likely offending agent, after which the condition will resolve.
Prednisone has shown efficacy in hypersensitivity vasculitis and can be used if the vasculitis is severe, is causing discomfort of the skin or other organ damage, or if it is imperative that the agent be continued despite the reactions. Because this is not the case, discontinuing the offending agent remains the highest priority.
Antihistone antibodies occur frequently in patients with either systemic or drug-induced lupus erythematosus. This patient's disease is more consistent with hypersensitivity vasculitis without specific features of drug-induced lupus (for example, malar rash); however, even if drug-induced lupus were the likely diagnosis, discontinuing the offending agent would still be the highest priority.
Palpable purpura is a clinical diagnosis for which a skin biopsy is not generally needed. A skin biopsy could be useful in cases where the mechanism of the rash needs to be understood to facilitate diagnosis or treatment, or when the rash fails to resolve despite management. In this case, the cause of the rash is known, and management should consist of removal of the offending agent before any further work-up is considered.
Key Point
- Hypersensitivity vasculitis is caused by a hypersensitivity reaction to antigens such as medication or infection and typically resolves when the offending agent is removed.




