The role of a lifetime in medical education
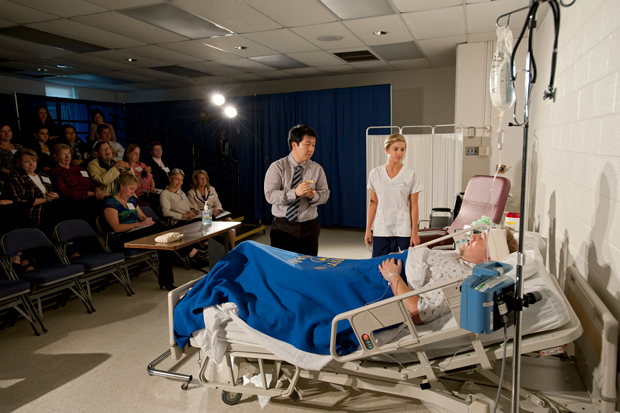
Standardized patients are used during medical school to ensure physicians develop competencies in communication and physical examination skills.
The role of the “standardized patient,” which turns 55 this year, has grown and adapted to medicine's changing landscape since its inception.
In 1963, neurologist and medical educator Howard S. Barrows, MD, recruited a woman at the University of Southern California (USC) to play “Patty Dugger,” a paraplegic patient with multiple sclerosis who was based on a real patient seen at Los Angeles County Hospital. Thought of as too “Hollywood” by many in neurology and medicine, Dr. Barrows' new educational tool eventually caught on and spread throughout the country.
“These methods were not always well received, but eventually people started to experiment and realized that standardized patients can give students feedback on clinical skills and on communication skills, all from a patient perspective,” said Karen Lewis, PhD, director of administration of the Standardized Patient Program and the Clinical Learning and Simulation Skills (CLASS) Center at the George Washington University School of Medicine and Health Sciences in Washington, D.C.
Today, standardized patients are used in the United States Medical Licensing Examination (USMLE) Step 2 Clinical Skills exam to test medical students and graduates on their ability to take medical histories, perform physical examinations, and communicate their findings.
Valuable lessons
The USMLE testing requirement greatly influenced many medical schools to establish their own standardized patient training programs, according to Daisy Smith, MD, FACP, ACP's Vice President of Clinical Programs.
“Many of these programs have evolved to make standardized patient programs a more useful tool for formative assessments that are valuable learning experiences,” Dr. Smith said. “They provide feedback in a low-stake setting where you don't have a sick patient or worried family hanging in the balance.”
Although initially programs had a checklist or “laundry list” of questions that the students had to ask the patient, many of them have evolved so that the checklist is shorter and students have to proceed in a more logical and patient-centered manner, according to Andrew R. Hoellein, MD, MS, FACP, associate dean for student affairs at the University of Kentucky in Lexington.
At the University of Kentucky, standardized patients are used to ensure other competencies as well, such as counseling of parents in the case of a pediatric patient or a psychiatric case, Dr. Hoellein said.
“We also want to make sure that students can take what they get from a history and a physical and apply it,” he said. “These interactions help them to start to work on medical decision making.”
As students advance in their training, they are faced with more challenging interactions, Dr. Lewis agreed.
“They have to learn to take a sexual history, or to take a history with a child and a parent,” Dr. Lewis said. “They have to learn how to break bad news to a patient, or tell someone that they have made a mistake.”
Role of the ‘patient’
Standardized patients are actors in some cases, or sometimes just people with an interest in health care. But all standardized patients need to know their script well and be able to act out the signs or symptoms of certain conditions, Dr. Hoellein said. They often learn a personal background, history of present illness, relevant medical history, family history, a social history, current medications, and how to respond to certain portions of a physical exam.
“Obviously, certain conditions cannot be acted out, like a heart murmur or pneumonia, but they can have neurologic symptoms or psychiatric symptoms,” he said.
One of the biggest challenges with standardized patients is ensuring reliability. Although patients are allowed to respond with emotion, they have to respond in relatively the same way to the same questions put forth by every medical student they see, Dr. Hoellein said.
In some cases, a mistake made by the standardized patient could jeopardize the intended lesson of the interaction, Dr. Lewis said. For example, one standardized patient was playing the role of someone who had recently developed diabetes, a woman in her 50s who was having trouble sleeping and starting to wake in the night to use the bathroom. In her social history, the woman had been widowed for two years and was just starting to date again. However, in the interaction with the medical student, the standardized patient elaborated on this history by adding that she was dating someone much younger and having the time of her life.
“It makes a great story, but an intelligent student might start to think about taking a sexual history and doing some patient education,” Dr. Lewis said. “As a result, the student did not get to demonstrate their knowledge of diabetes.”
Formative feedback
Immediate and formative feedback is one of the most important aspects of the innovative Healthcare Theatre program at the University of Delaware, co-founded by Amy Cowperthwait, RN, MSN, ACNS-BC, coordinator for the Adult Health Simulation Resource Center, and its director, Allan Carlsen.
Healthcare Theatre is a partnership between the College of Health Sciences and the College of Arts and Science that provides participants with an interprofessional and interdisciplinary education opportunity. Any student, including those studying to be health care professionals, can enroll in the program and train to become simulated performers such as patients, family members, or other clinicians, according to Ms. Cowperthwait.
Once enrolled, students participate in out-of-class preparation, improvisational workshops, and varied role portrayals throughout the semester. Students are given a script with pages of information about who their “patient” is and participate in dress rehearsals to ensure a level of standardization throughout the program.
“They have to embody this character and represent them during the simulation,” Ms. Cowperthwait said, adding that the experience also allows students to see illness and health care through the eyes of a patient.
Participants are also taught techniques for providing feedback to the health care learners from a patient perspective. After each interaction, the patient, student, and instructor meet to “debrief,” ask questions, and provide feedback on the interaction.
“Our focus is on peer-to-peer feedback, and that is something that this generation of students needs … immediate feedback,” Ms. Cowperthwait said. Ms. Cowperthwait stressed that it is important for future clinicians to know that patients' voices must be heard. To do that, they have to learn and be practiced in patient-centered communication techniques.
At the University of Delaware, health care students learn these techniques in the didactic portion of their coursework, Ms. Cowperthwait said. They then practice them during simulation and receive feedback from the “patient” and instructors.
“This cycle is repeated three times in the course of one semester and then reinforced in the subsequent semesters through simulation education,” she said. “That way it is not a theory to be memorized for an exam, rather a model for how to integrate patient-centered communication and seek feedback from ‘patients' from the beginning that they refine over the course of their prelicensure learning.”
Future directions
According to Dr. Hoellein, the role of the standardized patient in medical education is likely to expand, with a focus on compentency-based medical education. He feels the field is moving more toward entrustable professional activities, or unsupervised actions entrusted to the trainee, in order to ensure that students are capable of meeting milestones at certain points of their training.
“We'll have to be able to say that they are competent interviewing a patient at point X, physical examination at point Y, complex counseling at point Z, etc.,” Dr. Hoellein said. “Standardized patients are in a great position to help medical educators assure these competencies, as it is difficult for physician observers to be standardized and have the time for this.”
Dr. Smith sees the field of standardized patients expanding through the combination of human patients with technology.
For example, there is technology available that will allow medical students to practice ultrasound techniques that combine standardized patients with stored ultrasound images to simulate abnormal findings like heart failure or gallstones.
“We are also beginning to see more wearable technology that can be strapped to the standardized patients,” Dr. Lewis said.
At the University of Delaware, Ms. Cowperthwait and colleagues spun off the company Avkin, which created a line of wearable technology that is designed to maximize realism in the doctor-patient simulation. Wearable technology is designed to go on top of a live person and simulate certain medical situations.
With the Avkin product, standardized patients watch a 15-minute training video to explain how they should respond and react when wearing the technology. The wearable is equipped with sensors that trigger a vibration in the strap of the device that signals the patient to respond at the appropriate time with the appropriate reaction. The patient then gives an authentic simulation and can provide patient-centered feedback during the debrief, Ms. Cowperthwait said.
Another example of wearable technology is from Cardionics, which makes a product called the SimShirt that simulates physiological conditions and tests students' diagnostic and procedure skills, according to the Cardionics website.
Despite technological advances, however, the focus on the patient-physician relationship remains the most important aspect of standardized patient programs, Dr. Smith said.
“Although there are these technology mash-ups, I do not think we are ever going to get rid of the human piece of it,” she said. “There is a lot of really valuable information that our real-life patients have to teach clinicians of the future.”