MKSAP Quiz: 1 day of visual problems
A 55-year-old man is evaluated for a 1-day history of seeing flashing lights, “squiggly” lines, and floating objects in his left eye followed by loss of vision at the outer periphery of the eye shortly after having breakfast this morning. He now describes seeing what looks like a curtain coming down in that location. He has myopia requiring prescription glasses.
On physical examination, vital signs are normal. Vision in the right eye is 20/100 uncorrected and 20/40 with glasses. Vision in the left eye is 20/100 uncorrected and 20/40 with glasses. Pupils are equally reactive to light and accommodation. There is no conjunctival injection. Findings on funduscopic examination are shown.
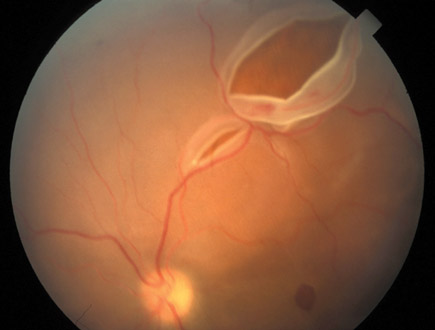
Which of the following is the most likely diagnosis?
A. Central retinal artery occlusion
B. Central retinal vein occlusion
C. Ocular migraine
D. Retinal detachment
E. Temporal arteritis
Answer and Critique
The correct answer is D: Retinal detachment. This question can be found in MKSAP 16 in the General Internal Medicine section, item 29.
This patient presents with symptoms consistent with a retinal detachment. Retinal detachment occurs predominantly in myopic patients and is a separation of the retina from underlying retinal epithelium and choroid as fluid from the vitreous cavity enters a tear in the retina and dissects underneath the retina. As with this patient, patients may experience floaters, squiggly lines, flashes of light, and then a sudden peripheral visual defect, appearing as a black curtain that progresses across the visual field. Funduscopic examination usually visualizes the tear and folding of the retina. Treatment is surgical. Prognosis depends upon the extent of the tear and time to surgery, so early recognition and emergent referral are crucial.
Central retinal artery occlusion is marked by painless loss of vision and occurs most frequently in the elderly. It is usually caused by emboli or thrombosis. Examination demonstrates a pale fundus with a cherry-red fovea (accentuated by the pale background).
Central retinal vein occlusion is characterized by abrupt monocular visual loss, and may present with transient episodes of monocular blindness, which can last 2 to 4 hours, longer than is typical for transient arterial retinal ischemia. Patients may report cloudiness of vision rather than frank visual loss. Examination of the retina will show congested, tortuous veins; retinal hemorrhages; and cotton wool spots in the area of the vein occlusion.
Ocular migraine, with or without headache, can cause floaters and squiggly lines but would not cause a visual field defect or a retinal tear and folding seen on funduscopic examination.
The most common presenting symptom in patients with temporal arteritis is a new headache, which this patient does not have. Although visual loss can be sudden and irreversible in the setting of temporal arteritis, it is not preceded by floaters, squiggly lines, or peripheral field defects.
Key Point
- Patients with a retinal detachment may experience floaters, squiggly lines, flashes of light, and then a sudden peripheral visual defect, appearing as a black curtain that progresses across the visual field.




