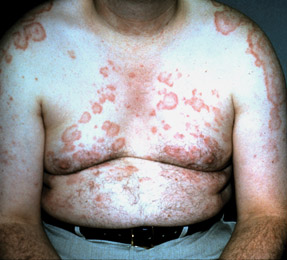
Lupus presentation may be an ‘imitator’
Lupus can involve multiple organ systems and shares the same, sometimes nonspecific presentation as other conditions. But a diligent internist##mdash;an “excellent generalist” in the words of one expert##mdash;can pick up on the correct diagnosis.
Systemic lupus erythematosus is a diagnostic challenge. It's insidious, and although the first sign to come to mind might be the telltale sun rash, symptoms can be vague and overlap with other diseases such as chronic fatigue syndrome, fibromyalgia, or rheumatoid arthritis.
“Several diseases are known as ‘the great imitators,’ and lupus is one of them, because it involves multiple organ systems and not every patient has the same presentation,” said Chaim Putterman, MD, chief of the Division of Rheumatology at Montefiore Medical Center and Albert Einstein College of Medicine in New York. “Initial symptoms can be nonspecific, such as fatigue, muscle pain, joint pain, and a general feeling of being unwell—nothing that clearly differentiates lupus from garden-variety complaints internists may hear.”

Because the initial symptoms can be so vague, internists tend not to think of lupus, said Marianthi Kiriakidou, MD, associate professor of medicine at Thomas Jefferson University and director of the Jefferson Lupus Center in Philadelphia.
“Often, if there are no other markers than inflammation, patients with fever will get several rounds of antibiotics [from an internist] before the internist thinks something else might be going on,” Dr. Kiriakidou said.
Yet internists may be uniquely positioned to shed light on a diagnosis, said Dr. Putterman. “In a fragmented health care system, patients may be seen by many doctors—hematologists, nephrologists, neurologists, obstetricians, and so on. Sometimes you need an excellent generalist to put everything together to say it's one disease.”
Screening
According to the Lupus Foundation of America, more than 90% of people with lupus are women, typically between the ages of 15 and 44.
“This is not to say that we don't see lupus in males, and there are limited studies and data on this, but it tends to happen either in their teens or when they are older than 50,” said Dr. Kiriakidou, who added that patient demographics should play a role when internists are assessing the possibility of lupus.
Race and ethnicity can also help determine the likelihood of lupus, as can family history, Dr. Kiriakidou added. The Foundation notes that lupus is more common in African-Americans, Hispanics, Asian-Americans, Native Americans, Native Hawaiians, and Pacific Islanders than in whites. The Foundation estimates that people who have relatives with lupus have a 5% to 13% chance of developing the disease themselves.
The most recent criteria for classifying lupus were developed by the American College of Rheumatology (ACR) and were published in the September 1997 Arthritis & Rheumatology. Although they were designed to classify patients for clinical trials, they are sometimes used in practice to help diagnose patients suspected to have lupus.
They consist of 11 items, of which 4 must be present for a classification of lupus. Of those 4, 1 must be a positive test result for autoimmunity. The 11 criteria are malar rash, discoid rash, photosensitivity, oral ulcers, arthritis, serositis (pleuritis, pericarditis), kidney disorder (protein or cellular casts in the urine), neurological disorder (seizures or psychosis), blood disorder (anemia, leukopenia, lymphopenia, thrombocytopenia), immunologic disorder (anti-DNA or antiSm or positive for antiphospholipid antibodies), and abnormal antinuclear antibody (ANA).
In a paper in the August 2012 Arthritis & Rheumatology, the Systemic Lupus International Collaborating Clinics (SLICC) group revised and validated the ACR SLE classification criteria, based on evidence from 1,400 patients and controls. The revision classifies a patient as having lupus if the patient has biopsy-proven lupus nephritis with ANA or anti-dsDNA antibodies or if the patient satisfies 4 of the ACR's diagnostic criteria, including at least 1 clinical and one immunologic criterion. Michelle Petri, MD, director of the Johns Hopkins Lupus Center in Baltimore and co-author of the SLICC group's paper, emphasized that SLICC is meant for classification, not diagnosis.
The ACR agreed this year to support a collaboration of North American and European lupus investigators on a project to develop new classification criteria for SLE, largely because of the need to more easily classify patients with early disease and better distinguish SLE from nonautoimmune conditions, said Amy S. Miller, senior director of quality for ACR.
When patients meet some criteria but not enough for a diagnosis, they should be monitored closely, said Gary L. Bryant, MD, FACP, vice chair for clinical affairs and associate professor of medicine in the Division of Rheumatic and Autoimmune Diseases at the University of Minnesota Medical School in Minneapolis.
“Early on, some patients may not qualify for a definitive diagnosis. They meet 3 of the criteria, not 4, so we follow along with the primary care physician for a while, calling what the patient has an ‘undifferentiated connective disease,’” said Dr. Bryant.
The autoimmune tests in the ACR criteria include the ANA test. Experts agree there are several caveats with this test.
“Just because it's positive, that doesn't mean the patient has lupus,” said Dr. Kiriakidou. “The ANA is a marker of autoimmunity but not necessarily of autoimmune disease. It will just tell us that the immune system is activated against the body. In the context of the right clinical presentation and other labs, it contributes to the diagnosis but is not itself enough for a diagnosis.”
According to an article in the October 2013 Annals of Internal Medicine by Dr. Kiriakidou and her colleagues, the ANA produces false positives in 3% to 5% of healthy individuals or patients with other autoimmune or infectious diseases.
“Because of the high percentage of false positives, make sure you don't do the ANA test for the wrong reason,” said Dr. Putterman. “For example, if you take 100 patients with back pain as a major presentation, 5% to 10% of them may be ANA-positive. You don't want to tell someone with lumbosacral pain that they have lupus. Only use the ANA in patients that have a moderate to high risk of autoimmune connective disease.”
Dr. Bryant noted that the ANA is more suited to ruling lupus out than in. “The chance that someone has lupus but a negative ANA is less than 10%. If the patient is negative, think 3, 4, or 5 times about diagnosing the patient with lupus.”
Internists who are ready to make a diagnosis of lupus should consult with a rheumatologist, said Dr. Putterman. “It's very important for there to be an initial referral to confirm the diagnosis. Then once the diagnosis is confirmed, I would view management as a partnership between internist, rheumatologist, and the patient,” he said.
Managing lupus
The experts agree that complex cases involving active disease, life-threatening disease, multiple organs, or comorbidities such as heart failure should be managed primarily by a rheumatologist.
“Most internists would not be comfortable initiating therapy in patients in active disease, as it can be severe and the drugs and medications that are used are cytotoxic, immunosuppressive, and associated with potentially dangerous side effects,” said Dr. Putterman.
These drugs include mycophenolate mofetil, azathioprine, methotrexate, cyclophosphamide, cyclosporine, tacrolimus, belimumab, and rituximab.
However, internists could be comfortable with long-term management, Dr. Putterman said. “Lupus patients need a lot of regular follow-up even if the disease is apparently clinically inactive. Those with active disease may need to be seen once every few weeks for 2 or 3 months.” He also noted that internists play a crucial role in watching out for infections in patients on immunosuppressive drugs because they often see infections in other parts of their practices.
Dr. Bryant agreed. “Once a treatment plan is in place, a lot of the monitoring can be done by the internist with occasional visits to the rheumatologist just to weigh in on whether there is a need for any changes in disease management.”
Geography matters, particularly with immunosuppressive drugs, which need to be monitored every few weeks. “It may be more convenient for a patient to see an internist in rural areas or in areas where there are few rheumatologists. I rely on patients having an excellent relationship with their primary care providers,” said Dr. Bryant.
Milder cases of lupus may offer internists an opportunity to take the lead in disease management, said Deana Lazaro, MD, chief of the rheumatology section at the VA New York Harbor Healthcare System in New York. “These would be limited to skin manifestations, arthritis, and constitutional symptoms,” she said.
Dr. Lazaro noted that treatment in mild cases can be as simple as NSAIDs, but the mainstay is hydroxychloroquine.
“It's ideal because it treats joint symptoms and constitutional symptoms and has other health benefits, such as a positive effect on glycemic parameters and lipids, as well as the risk of lupus flare,” Dr. Lazaro said. She added that hydroxychloroquine requires regular eye tests, another area of care internists can oversee.
While lupus can affect every major system, the kidneys are particularly vulnerable. The Lupus Foundation of America estimates that 40% of adults and nearly 66% of children with lupus will develop kidney complications that require medical evaluation and treatment.
Patients with lupus are at increased risk of cardiovascular events, as well. A paper in the August 2005 Nature Clinical Practice Cardiovascular Medicine noted that risk of heart attack rises 50-fold in women between 35 and 44 who have lupus.
Because lupus is a head-to-toe disease, internists can help their patients minimize risks of complications by ensuring that they receive appropriate medication-related monitoring and the basic care and education they need.
Dr. Kiriakidou's paper in Annals noted that routine laboratory testing should include a complete blood count, basic metabolic panel, and urinalysis during follow-up visits and that all patients with lupus should receive flu and pneumonia shots.
The Lupus Foundation of America notes that the overall risk of cancer is 10% to 15% higher in people with lupus. A paper published in the May 2013 Journal of Autoimmunity noted increased risk of cancers such as non-Hodgkin's lymphoma, leukemia, and cancers of the vulva, lungs, thyroid, and possibly liver.
“Preventive cancer screening should be up to date,” said Dr. Kiriakidou. “Everything from Pap smears to mammograms to colonoscopies should be done according to prevailing guidelines.”
Flares and corticosteroids
Corticosteroids are part and parcel of lupus treatment, and internists should not shy away from them when the patient is having a flare, said Dr. Lazaro. “It's important to use enough for the condition you are treating. If you use too little, the autoimmune process will continue, and then you end up using more in the long run. The idea is to hit it hard in the beginning, then taper as rapidly as possible and switch to a steroid-sparing agent.”
Dr. Petri agreed. “Our goal is to get everyone off the steroids as soon as possible, or at least to less than 6 mg. Long-term use of corticosteroids increases the risk of permanent organ damage later and increases the risk of cardiovascular events.”
Internists can take the lead on talking to their patients about the dangers of continued prednisone use, said Dr. Putterman.
“Some patients take more prednisone than we would like, or they take it for a few weeks, stop suddenly, then start again, which is potentially life-threatening,” said Dr. Putterman. “But internists are familiar with drugs like prednisone from other patients who are on it for various other reasons and are vital in ensuring that the patient is taking this class of medications correctly.”
Dr. Kiriakidou noted that despite its risks, prednisone is the preferred way to quickly suppress the inflammatory process. “Some medications take 4 to 6 weeks for full effect, and you don't want a patient to have to wait a month and a half with swollen joints and joint pain to get relief,” she said. “Just remember that it's a bridge therapy.”