MKSAP Quiz: Emergency visit for chest pain
A 66-year-old man is evaluated in the emergency department for chest pain. He describes a sharp pain in the midchest that does not radiate. The pain began suddenly at rest and has persisted for approximately 40 minutes. He has hypertension treated with amlodipine.
Temperature is 37.4°C (99.3°F), blood pressure is 180/80 mm Hg in the left arm and 200/80 mm Hg in the right arm, pulse rate is 110/min, and respiration rate is 18/min. BMI is 32. Pulse oximetry shows oxygen saturation of 98% on ambient air. A normal carotid upstroke without carotid bruits is noted, jugular venous pulsations are normal, and normal S1 and S2 are heard. A grade 2/6 early diastolic murmur is heard at the left sternal border. Lung fields are clear, distal pulses are normal, and no peripheral edema is present.
Laboratory studies:
| Hematocrit: | 40% |
| Platelet count: | 220,000/µL (220 × 109/L) |
| Creatine kinase: | 100 units/L |
| Creatinine: | 1.6 mg/dL (141 µmol/L) |
| Troponin I: | 0.05 ng/mL (0.05 µg/L) |
| Myoglobin: | 40 ng/mL (40 µg/L) (normal range, 0-90 ng/mL [0-90 µg/L]) |
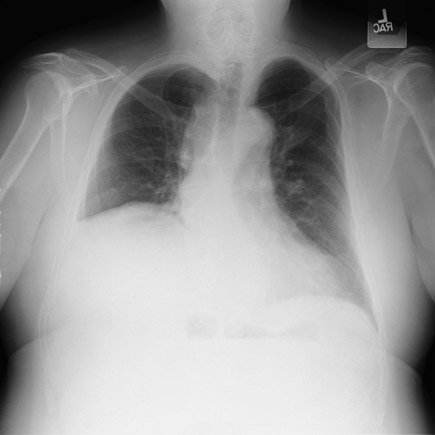
Electrocardiogram shows sinus tachycardia at 110/min, with nonspecific ST- and T-wave changes in the lateral leads. Chest radiograph (portable film) is shown.
Which of the following is the most appropriate diagnostic test to perform next?
A. Chest CT
B. Electrocardiography with posterior leads
C. Transthoracic echocardiography
D. Ventilation-perfusion scanning
Answer and critique
The correct answer is A: Chest CT. This question can be found in MKSAP 16 in the Cardiovascular Medicine section, item 50.
A CT scan of the chest should be obtained. A prudent approach to patients with acute chest pain focuses the initial evaluation on six potentially lethal conditions (the “serious six”): acute coronary syndrome, pericarditis with tamponade, pulmonary embolism, pneumothorax, aortic dissection, and esophageal rupture. Physicians must rapidly evaluate patients and exclude each of these conditions to initiate appropriate therapy. In this patient with acute-onset chest pain that began at rest, upper extremity blood pressures are asymmetric, there is an early diastolic murmur consistent with aortic regurgitation, and the electrocardiogram (ECG) shows no ST-segment elevation. The chest radiograph shows a widened superior mediastinum and a right pleural effusion. These findings are consistent with an acute aortic dissection. The right pleural effusion is most likely a hemothorax from the acute aortic dissection. CT of the chest would be the most efficient means to establish the diagnosis prior to proceeding to emergent surgery.
Posterior ECG leads (V7 through V9) can be useful in the diagnosis of an isolated posterior wall ST-elevation myocardial infarction (STEMI). An isolated posterior wall STEMI accounts for approximately 7% of all STEMIs and should be considered in patients presenting with anginal chest pain and nonspecific findings on a standard 12-lead ECG. Given that the duration of the patient's chest pain is 40 minutes, however, the normal myoglobin and troponin I levels argue against an acute coronary syndrome as a cause for the symptoms.
For a patient with a presumed ascending aortic dissection, imaging of the proximal ascending aorta can be difficult and, therefore, transthoracic echocardiography is not the imaging method of choice. In contrast, transesophageal echocardiography has high diagnostic accuracy for an ascending aortic dissection and, in some medical centers, is the imaging method of choice in unstable patients for whom transportation to the CT or MRI scanner may not be safe.
Although this patient's description of chest pain could be consistent with a pulmonary embolism, this diagnosis cannot explain the discrepant arm blood pressures or diastolic murmur; therefore, ventilation-perfusion scanning is not the most appropriate test.
Key Point
- In a patient presenting with acute chest pain, the life-threatening diagnoses of pulmonary embolism, acute aortic dissection, acute coronary syndrome, pericardial tamponade, pneumothorax, and esophageal rupture must be rapidly evaluated for and excluded.