Patients with diabetes facing vision loss at ever-earlier ages
Just as diabetes is affecting younger populations, so are its consequences. Childhood obesity can translate into diabetic retinopathy in patients in their 20s, which requires a response from the primary care community.
How do you convince twenty- or thirtysomething patients with type 2 diabetes that they may already be suffering from an eye disease—even though they don't perceive any visual loss—and then ensure follow up?
These are key challenges for internists now seeing patients with obesity- and metabolic syndrome-related conditions that their patients may have had since childhood. Diabetes-related nonrefractive visual impairment is increasing in young adults, a population traditionally not thought to be at risk for eye disease, according to a recent study published in the Journal of the American Medical Association.
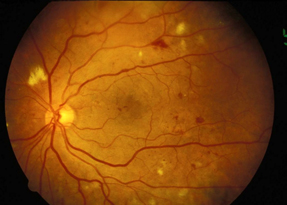
Already those trends are being seen in practice. While it's not surprising that Doron Schneider, MD, FACP, has patients as old as 89 on insulin and metformin, now, he said, he has patients on that regimen who are as young as 20. And Anne Peters, MD, FACP, says patients in her east Los Angeles clinic, who typically have limited access to care, are showing a disturbing trend.
“I'm seeing severe retinopathy in 20- and 30-year-olds. It's disconcerting because it's a preventable complication,” she said.
It can also have a profound impact on young adults now facing the prospect of expensive treatment and/or lifelong vision loss that can impact their ability to work.
“Think about being told you have significant loss in vision when you're 28 years old,” said Daniel Lorber, MD, FACP, associate director of the Lang Center for Research and Education and director of endocrinology at the New York Hospital Queens in Flushing, N.Y. “[These patients] are going to be angry and scared. This is a horror.”
Internists need to take action now to raise awareness of prediabetes, to find opportunities to make treatment inroads, and to provide one-stop shopping for a patient population that is not likely to be regularly visiting their internist's office, said Dr. Schneider, chief of patient safety and quality officer at Abington Memorial Hospital in Abington, Pa.
Doing so can begin to stem what David S. Friedman, MD, MPS, PhD, co-author of the Dec. 12, 2012, JAMA article, called a significant public health concern. “This is the beginning of a tidal wave of diabetic eye disease and retinopathy,” he warned.
Growing problem
It makes intuitive sense that the problems associated with patients who have diabetes for at least 10 years would begin to show up in younger patients given increasing childhood weight issues. Now the JAMA study results show just how serious the problem is already and why efforts to address the issue can't come too soon.
The study, which used data from the National Health and Nutrition Examination Survey (NHANES), found that nonrefractive visual impairment in adults over 20 increased 21% from the 1999-2002 survey period to 2005-2008, from 1.4% to 1.7%. Some populations seemed at particular risk, such as Mexican Americans. Patients at greater risk also were poor, lacked health insurance and had less education.
However, those risks were similar in the previous survey. By eliminating other factors, the researchers attributed the jump to longer duration of diabetes, said Dr. Friedman, professor of the Dana Center for Preventive Ophthalmology at the Wilmer Eye Institute at Johns Hopkins in Baltimore.
“We didn't look at each person's [eyes] to see what was going on in there ... but all associations support the finding,” he said. For example, he noted that nearly 1% of the 20- to 40-year-old group had type 2 diabetes for 10 years or more and that other studies have shown retinopathy to be associated with uncontrolled blood glucose and blood pressure.
He said the results make it more imperative than ever for patients to receive general care in order to improve their blood glucose, and to routinely screen their vision. The American Diabetes Association standard of care is for all type 2 diabetes patients to have a retinal exam at diagnosis, then every year thereafter.
Challenges and solutions
Prevention is key even though treatments can be very effective, especially the earlier they're started. In fact, retinal lasers, medications (e.g., ranibizumab and other pharmacologic agents for macular edema), and surgery are 90% effective in preventing severe vision loss, according to Charles C. Wykoff, MD, PhD, of Retina Consultants of Houston.
The frustrating part, he said, is that because retinopathy seems to be initially asymptomatic, significant damage often occurs before the patient notices or seeks medical attention.
The problem really begins with handoffs of at-risk adolescents, said Nathaniel G. Clark, MD, FACP, an endocrinologist with Emerald Physicians in Hyannis, Mass. There can be a gap of 10 years where the patient has been healthy and feels too young to see an internist but too old to remain with a pediatrician. During this time, there can be poor control of blood pressure and glucose, leading to an increased risk of complications.
“Young adults often get lost in the transition from pediatric to adult care. It can be hard to keep the connection,” said Dr. Peters, professor of medicine at the Keck School of Medicine at the University of Southern California and director of its clinical diabetes program. Having clinicians share information and provide support to these young patients can help address the problem, she said.
Experts also say internists have to adjust, from thinking about vision issues as pertaining to just older patients with glaucoma or cataracts to more aggressively diagnosing and treating their younger patients.
“We're accustomed to thinking of those patients as just talking about smoking, safe sex and alcohol, not necessarily about blood pressure, cholesterol and diet,” Dr. Clark said.
One way internists can do a better job screening is by piggybacking diabetes screening and blood pressure control when young patients come in for some other symptom, such as a shoulder sprain, Dr. Schneider said.
While internists may be able to see obvious vision problems in these patients, they should refer diabetes patients to a specialist, said Dr. Peters.
She acknowledged that can be a problem because follow-up can be a major stumbling block for many reasons. Her clinic in east Los Angeles, which was funded by a county Medicaid grant, addressed the issue by becoming a one-stop shop. Patients see a doctor and nurse, get their eyes checked by an on-site optometrist, and have lab results available online 20 minutes later.
Other tips
There's reason for optimism. K. Bailey Freund, MD, a retina specialist with Vitreous Retina Macula Consultants of New York and a clinical spokesperson for the American Academy of Ophthalmology, has seen improved retinas in patients with drastic weight loss, for example. But the pressure's on internists to figure out how to work with these younger patients to better control their diabetes and potential for existing retinopathy.
Here are some ideas from those who spoke with ACP Internist:
Screen for prediabetes. Ask more questions, such as, “Did you pass your driver's test?” Provide a booklet with instructions on how to reduce risks.
Educate patients. Once the diagnosis is made, make sure patients understand the goals of care and the relationship between diabetes and eye problems. That will empower them to be engaged partners in their care. “I don't take care of diabetes,” Dr. Lorber said. “I help people take care of it.”
Use team-based care. Standardize what each staff member is doing in the exam room and have everyone work to the top of his or her license. Have the nurse or medical assistant note that the patient has diabetes and the date of the last eye exam, and discuss goals. The doctor can then deal with the acute, more complex decision making.
Refer to a specialist and follow up. Any patient with prediabetes, diabetes or hypertension should see an ophthalmologist. Then be sure the specialist gives you a report. Dr. Clark said he works on having close relationships with his local eye care professionals and regularly communicates with them. “We do a good job so patients know somebody is watching,” he said.
Consider telemedicine. Get connected electronically with your local ophthalmologists by sending eye photos of high-risk patients to a retina specialist for consultation. Dr. Wykoff said that while currently telemedicine cannot replace a comprehensive ocular exam, it may identify high-risk patients who could benefit from immediate consultation.
The best answer?
Younger, typically healthier patients present a unique challenge because they don't see the need for a patient-centered medical home (PCMH). They may be more likely to, for example, go to a retail clinic, Dr. Schneider acknowledged. However, he said the medical home is the ultimate solution for this population and this issue because it is more likely to reach out to patients with a diabetes diagnoses and ask them to come in for any needed services such as labs.
A PCMH would use disease registries to run a list of patients who are diabetic but haven't received an eye exam. Then the practice could send e-mails or postcards or make telephone calls for exam or lab reminders. ACP's Medical Home Builder offers resources that will help identify patients and track results.
Dr. Clark uses his registry to track his patients' eye exams and findings and sends letters at the beginning of every month to patients who haven't been seen in six or nine months. While they may have received reminders from their dentist or even auto mechanic, they usually say they've never received one from a doctor. “But it's what the health care system needs to do if we're to have an impact,” he said.
Tighter adherence can result in tighter hemoglobin A1c control, which in turn holds the promise of a huge payoff.
“I can confidently tell a patient if you watch your weight, diet, blood pressure and sugars you can have vision for a very long time,” Dr. Freund said.