Letters to the Editor
Readers respond about bedside vs. scanning and how to take blood pressure.
More bedside, less scanning
The case history presented in Mindful Medicine [“Priming to diagnose an atypical case, avoid representativeness,” ACP Internist, July/August 2011] was fascinating to read, but it left me with some questions and the need for some comments. Firstly, I wonder what was the need for a head CT scan on the patient's initial presentation with fatigue and weight loss. I could not find any symptoms or signs relating to the head or the nervous system. As noted, the patient even went on to have sinus surgery, all the while the grave symptom of weight loss was sidelined and evidently blamed on depression, for which he received antidepressants.
Then, there is the question of Helicobacter pylori diagnosed by the gastroenterologist, who did not just stop at upper endoscopy but performed colonoscopy, which was not indicated at that time. What was he/she looking for, I wonder. There were no symptoms of the upper gastroenterological distress that would prompt hyperacidity and a legitimate suspicion of an ulcer or gastroesophageal reflux disease. It is also possible that the H. pylori was an incidental finding causing the patient no symptoms or morbidity, as we all know that all H. pylori carriers are not infected.
I agree that a cosyntropin test was indicated after adrenal cortical failure was suspected, but I presume the basal cortisol levels were done first. I contend it should not have to take an endocrinologist to think of Addison's or even multiple endocrine syndrome in this patient, nor a gastroenterologist to think of hemochromatosis. I think any well-trained and observant internist could have diagnosed this patient's adrenal insufficiency.
Recently I was misdiagnosed in a hospital setting. I presented with severe upper abdominal pain, anorexia and nausea due to esophageal ulceration because I had a violent emesis while in the emergency room, induced by drinking a liter of contrast agent for a worthless abdominal CT scan. The endoscopy showed the “ulcer,” which most likely was a Mallory-Weiss tear. The hematemesis stopped as suddenly as it came, happened just once and with no malena. I suffered three more days of agony on ineffective proton pump inhibitors until readmission to the hospital and a hepatobiliary iminodiacetic acid scan revealed a non-functioning and dramatically enlarged gall bladder, the cause of my initial symptom. After an urgent laparoscopic cholecystectomy I returned to health, seven days postoperatively.
I think nowadays there is a serious lack of needed clinical bedside skills, and there is excess enthusiasm to perform procedures and rely on them for diagnosis. Clinicians are losing their integrative diagnostic outlook and allowing themselves to be misled by isolated tests.
Byravan Viswanathan, FACP
Gettysburg, Pa.
How not to take blood pressure
I enjoy ACP Internist's good editorial work, but while I appreciated the article on the
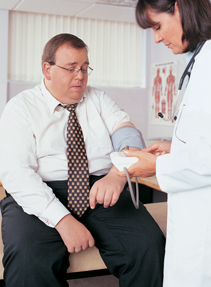
difficulty doctors have with treating obesity [“Tread lightly: Discussing obesity difficult for internists,” ACP Internist, July/August 2011], I have problems with the accompanying stock photo on page 10. I would suggest that the picture could be captioned “How not to take blood pressure.” The patient's sleeve is rolled up and constricts the upper arm (because he is obese). Also, the cuff is placed over the bend of the elbow, and guidelines indicate that it should be placed about the level of the heart, not below it. The picture, unfortunately, reminds me of some of the old doctor shows on TV, where the actor would put a stethoscope in his ears the “wrong” way, or put an X-ray on the view box backwards.
Loyd Wollstadt, FACP, MSc
Rockford, Ill.




