Project ECHO expands the reach of primary care
To improve local care of hepatitis, Project ECHO uses videoconferencing and case-based learning to connect front-line primary care physicians with skilled and knowledgeable specialists.
In 2003, hepatitis C virus (HCV) infection was a growing problem in New Mexico. Fewer than 5% of the state's estimated 30,000 community-dwelling people with hepatitis C and none of its 2,300 prisoners with the disease were receiving treatment, according to Sanjeev Arora, FACP, a hepatologist and gastroenterologist at the University of New Mexico in Albuquerque. Primary care physicians weren't equipped to treat HCV infection, and the state simply didn't have enough specialists to meet the demand.
“People seeking treatment would come more than 250 miles each way to see me, and sometimes they had to make up to 18 trips to be treated,” Dr. Arora said. “At times, there could be up to an eight-month wait to see me. In 2003-2004, there was not a single primary care physician treating hepatitis C in all of New Mexico.”
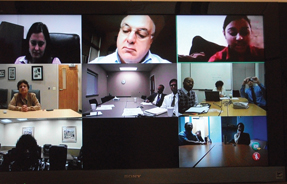
The solution, Dr. Arora thought, could be training primary care physicians to treat hepatitis C locally. To that end, he created Project ECHO (Extension for Community Healthcare Outcomes), an innovative model that uses videoconferencing and case-based learning to connect front-line primary care physicians with skilled and knowledgeable specialists.
The backbone of Project ECHO is based on four key ideas, according to Dr. Arora. The first is the use of technology, including multipoint videoconferencing and the Internet, which can leverage scarce health care resources that may only exist in large cities or at large academic health centers. Second is the use of a disease management model that focuses on improving outcomes by reducing variations in processes of care. Third is the use of case-based learning. Finally, Project ECHO uses a secure centralized database to monitor patient outcomes.
Primary care practices that are interested in joining must undergo a two-day orientation in Albuquerque, where they will learn more about the disease treatment protocol and much of the technology and case-based format used during telemedicine consultations with specialists. Next, they are assigned to a learning network with other primary care physicians and University of New Mexico Health Sciences Center specialists who will participate in weekly videoconference sessions to present and discuss cases.
This team of specialists will never see the primary care physicians' patients, but instead uses a guided practice model to slowly help the physicians operate with increasing independence as their knowledge of hepatitis C, skills in treating the disease, and self-efficacy increase.
“We found that clinicians learned best with the same kind of learning they had during fellowship and residency ... with mentors comanaging patients with them instead of trying to do it themselves by reading textbooks,” Dr. Arora said.
Immediate effects
According to the results of a study by Dr. Arora and colleagues published in June in The New England Journal of Medicine, this partnership of specialists with primary care physicians has had a great effect on hepatitis C in rural and remote New Mexico. When percentages of patients with a sustained virologic response and adverse events were compared, the treatment at Project ECHO sites was equivalent to that at the University of New Mexico's hepatitis C clinic.
“By learning from each other, learning by doing and learning from specialists, they rapidly become experts,” Dr. Arora said. “This NEJM study shows that these people can manage this disease as well as anybody who is a specialist can.”
In addition, participating physicians earn low-cost continuing education credits and are able to interact with colleagues with similar interests. In fact, in another study published in Hepatology in 2010, Dr. Arora and his colleagues found that those involved in the program had not only a significant improvement in knowledge and self-efficacy, but also more professional satisfaction and reduced professional isolation.
Spreading the word
Project ECHO is now being used for more than 10 different conditions in New Mexico: asthma, chronic pain, diabetes and cardiovascular risk reduction, high-risk pregnancy, HIV/AIDS, mental illness, pediatric obesity, rheumatology and substance abuse disorders. It's also being adapted by other medical centers, including at the University of Washington in Seattle and the University of Chicago.
John D. Scott, MD, is the principal investigator of Project ECHO at the University of Washington, the first project location outside New Mexico, which serves people across Washington, Alaska, Wyoming, Montana and Idaho—five states and three time zones.
The program also began with hepatitis C in 2009 at about five sites in western Washington, but now adds about five sites every six months, Dr. Scott said. A site may have two to eight clinicians joining. Since 2009, the Washington program has expanded its offerings to include integrated addiction and psychiatry and chronic pain.
“Washington recently passed legislation that requires patients on more than 120 mg of morphine a day to be reviewed by a pain specialist,” Dr. Scott said. “In this whole area [Washington], we had about eight chronic pain specialists and about 20,000 patients who were being prescribed high-dose opioids. For this new domain [chronic pain], we had about 20 sites sign up after only two months and anticipate getting up to about 60 sites by the end of the year.” (For more on nationwide hepatitis efforts, read the related article, “Primary care integral to new national viral hepatitis action plan.”)
The University of Chicago, meanwhile, began applying Project ECHO in 2010 to an underserved urban area, pairing with several federally qualified health centers to improve care of hypertension in the local African-American community.
“We conducted a baseline survey and a follow-up survey among participating and control physicians after the first 12 ECHO teleconferences,” said Christopher Masi, ACP Member, assistant professor of medicine in the university's Section of General Internal Medicine. “Although the data are early, we found there were increases in both hypertension management knowledge and hypertension management self-efficacy among those physicians who participated in the program versus no increases among those who did not.”
Both the University of Washington and the University of Chicago plan to further expand not only the number of project participants but also the disease states addressed. Six criteria qualify a disease state as adaptable to Project ECHO, according to Dr. Arora:
- 1. The disease is common.
- 2. The management of the disease is complex.
- 3. New treatments for the disease are emerging.
- 4. The disease has a high societal and economic effect.
- 5. Serious outcomes occur if the disease is left untreated.
- 6. There is existing effective treatment for the disease.
Get involved
How can clinicians interested in this program get involved?
“Call us!” said Dr. Arora. “In New Mexico, a physician can call us and we send a technology team out to set them up. They then have to attend a one- or two-day ‘orientation’-type visit, but we get them set up in a relatively short period of time.” (Contact information for Project ECHO is available online. )
Getting involved in Project ECHO in new locations may take a little more time and effort.
“Dr. Arora gave us protocols on conditions, advice on how to recruit sites and guidance on how to run clinics. Basically all the nuts and bolts of the operation,” said Dr. Scott. “We had frequent e-mail and phone exchanges, as well as live visits both [in Washington] and in New Mexico. The biggest issue was getting time into the very busy schedules of a lot of our primary care physicians,” Dr. Scott said.
To solve the time issue, video conferences were scheduled during lunch and included an agenda; participating clinicians were also eligible for continuing medical education credits. In Chicago, Dr. Masi resolved a similar issue by holding videoconferences at 8 a.m. Mondays before a clinic opens for the week.
Funding is also a potential obstacle. Currently, New Mexico's Project ECHO is funded with a three-year, $5 million grant from the Robert Wood Johnson Foundation's Pioneer Portfolio with additional support from the Agency for Healthcare Research and Quality, the New Mexico state legislature, the University of New Mexico and the New Mexico Department of Health.
“Dr. Arora has demonstrated that Project ECHO saves money,” Dr. Masi said. “States can definitely save money if individuals are treated for complex diseases by primary care physicians instead of by specialists at [academic medical centers].”
Dr. Masi said that although his Chicago program will continue to apply for funding support through grants, working to gain funding through the state may be the best long-term solution. And Dr. Arora believes that with time, insurance companies and state governments will adopt the model as a smart way of conducting business. Dr. Scott agreed.
“The holy grail is getting Medicare and Medicaid to buy into the program and support it with funding,” he said. “But that is the direction I see health care going ... more quality improvements, and not necessarily volume. That is where ECHO comes in by using best practices, reducing variation in care and reducing health disparities.”





