Rethinking the value of the annual exam
Patients expect it and internists won't let it go. But does the evidence support the need for the periodic health exam? Experts weigh in on the value of regularly seeing a patient on a preventive basis.
One constant in medical care is the persistent notion of the value of the annual physical. There's no strong evidence base for the periodic health exam (PHE), as it's now often called, as a discrete encounter, and no consensus on what it should include. But most patients expect it, and many internists are unwilling to let it go.
The chief cited rationale is that the annual offers a regular opportunity to address risk factors and health or life concerns.
“There's little evidence that a routine physical exam and a standard 20-30 item chemical panel improve outcomes,” said Allan Goroll, MACP, a professor of medicine at Harvard Medical School and practicing general internist. “However, there is substantial evidence that checking for and treating cardiovascular risk factors, preventable or curable cancers, STDs, depression and substance abuse are all evidence-based, high-value activities.”
Many studies confirm the value of tobacco and obesity counseling and the importance of blood pressure checks in disease prevention. Given the obesity epidemic, few internists would quibble with the U.S. Preventive Services Task Force (USPSTF) recommendation that adults should be screened at least every five years for high cholesterol, and more frequently if cardiac disease or risk factors exist. The PHE offers a chance to tackle these issues with patients.
“The PHE's value lies in its provision of opportunities for patients and physicians to address needed recommended prevention interventions in a given visit,” said Ebony Boulware, MD, associate professor of medicine and epidemiology at Johns Hopkins School of Medicine and lead author of a February 2007 Annals of Internal Medicine review on the PHE. “Because patients show up for that visit, internists may be more likely to ensure they've received all of the needed recommended screenings for that year.”
Studies have confirmed that patients who undergo an annual are more likely to receive cholesterol screening, Pap smears, gynecologic exams and fecal occult blood testing. According to Dr. Boulware's research, PHEs decrease patients' worry, which may benefit them and the patient-physician relationship, although more study on this issue is needed.
David Shih, MD, senior director of medical affairs for the American College of Preventive Medicine, cites another PHE value that isn't supported by evidence.
“The whole laying of hands on people is something a lot of primary care physicians see value in,” he said. “And for some it's a standard of care issue; it's what physicians feel they should be doing for all patients, so they do it.”
Evidence-based limits
Despite findings that some complete blood counts (CBCs), chemistry panels, thyroid checks, urinalysis, electrocardiograms and treadmill tests are of little or no value, many physicians still do them. Opponents of the traditional annual cite the AHRQ/Evidence-based Practice Center systematic review and the scant evidence .
Even those who think annuals aren't necessary acknowledge that asymptomatic patients should undergo preventive screenings and risk factor assessment in some preplanned encounter. Whether that's an annual or biannual dedicated visit, a series of scheduled shorter visits, or a screening tucked into an acute care visit is best determined by the internist based on practice resources and patient population.
But basing screening only on evidence can be difficult, Dr. Shih noted. He pointed out that the USPSTF, for example, can review only the data available, and it's not always comprehensive. “The task force is often limited in what it can say, and often intervals for screenings are poorly defined. That's a frustration for many physicians,” he said.
Mary Barton, ACP Member, USPSTF's scientific director, acknowledged the evidence gaps but noted that the Task Force has historically focused on clinical preventive services with more targeted outcomes. “It is extremely difficult to construct a framework for an evidence review that can successfully incorporate multiple outcomes. For example, in examining the effects of an annual physical one might want to consider effects on outcomes related to heart disease, cancer, depression, alcohol misuse, sexually transmitted diseases, etc.”
The USPSTF has made significant strides in recent years to make it easier for internists to sort through its recommendations. The Electronic Preventive Services Selector (EPSS) tool lets physicians quickly access screening recommendations for particular patients, and provides extensive detail on both clinical considerations and rationale.
The tool also provides ample information on services and screenings the USPSTF recommends against or for which there is insufficient evidence to make a recommendation for or against. This information, along with links to other materials for clinicians and patients, can be helpful in framing conversations to support shared decision making, explained Jan Genevro, PhD, a scientist with the Agency for Healthcare Research and Quality who helped develop the EPSS.
“The EPSS makes it possible for clinicians to show patients directly which services are and are not recommended. Many clinicians have found it helpful to share the EPSS results for a specific patient with that patient as the basis for developing a personalized prevention plan.”
Focused exam works best
Internists who choose to provide a structured annual visit should tailor the encounter to focus on the elements that matter, Dr. Goroll advised, and to focus cancer screenings on the ones “where interventions in the asymptomatic period make a difference in outcomes. That's melanoma, colon cancer and cervical cancer, lymphoma, and probably breast cancer and prostate cancer.” (The fallout of the release of USPSTF breast cancer guidelines will be addressed in ACP Internist's February issue.)
“It could be done in less than 30 minutes of physician time, if you're being truly evidence-based and have a team-based approached to the visit. Much of the work needn't be done by the internist,” Dr. Goroll said.
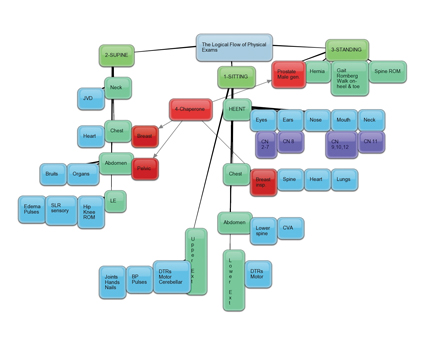
A mid-level team member could do the initial routine screening and identify issues that require attention by the physician, he said. “This approach preserves physician time for the necessary high-level inputs such as counseling and design of a personalized screening or management plan.”
In practices that use electronic medical records (EMRs) with trigger functions, focused visits and recommended screenings are easier to schedule, Allan Prochazka, FACP, professor of medicine at the University of Colorado Denver, said. He urged internists, whether they use EMRs or not, to consider personalized plans.
“For me, tailoring is where it's at,” Dr. Prochazka said. “To the extent that you can build it into their ongoing care it makes more sense than a separate visit. If I go to the doctor I don't want generic care, I want care for me that's also evidence-based.”
But that's not what happens in many primary care practices, Dr. Prochazka and fellow researchers found in a 2005 survey published in Archives of Internal Medicine. Nearly half of the physician respondents, despite evidence to the contrary, still believed in annual mammography, lipid panels, blood glucose levels, CBCs and urinalysis.
“In general, there's a bit of a disconnect,” he said. “Many patients wish for tests and think that's what a physical actually means. And many physicians think that the traditional annual is necessary and of proven value.”
Dr. Prochazka said that if internists were to move toward more tailored PHE visits and spend more time on lifestyle issues than on tests, patients would eventually accept that. “The things that we do become pretty salient to patients,” he said.
Ned Calonge, MD, MPH, chair of the USPSTF, also thinks that internists should spend more time counseling, since factors like physical activity, nutrition and tobacco use are important determinants of disease. Likewise, he added, many primary care physicians steer clear of discussing obesity, alcohol misuse and depression.
“We know that alcohol misuse problems can increase in the elderly, for example, but often we just don't ask,” he said. “The same thing occurs with obesity. It's remarkable, in surveys, how many patients say ‘My doctor never mentioned that my weight was a problem.’”
For internists seeking direction on where to focus their clinical screening efforts, Dr. Calonge offered a short list. “The heart disease cluster hypertension, lipid disorders, obesity and tobacco counseling are the things I think internists really should focus on,” he said.
Relationship-building important
All sources agreed that the evidence base shouldn't be the only thing dictating whether and how an annual is performed. It's hard to measure the value of a PHE in improving the doctor-patient relationship and getting patients to talk about personal issues that could affect their health, for example. But most internists believe that the PHE accomplishes both.
“Many internists like the periodic exam because it's a chance to put a little more time on the schedule, and sit down and actually get to know your patients,” said Michael Barr, FACP, ACP's vice president for practice advocacy and improvement. “Even if there are no acute concerns, or the chronic ones are well managed, it's a chance to cover material on preventive care that you might not have time to do in an acute care visit.”
Dr. Goroll concurred. “Not to be underestimated is the value of maintaining the doctor-patient relationship, as well as counseling for life stresses and personal issues that come up,” he said. “A lot of behavioral and mental health problems emerge during the annual visit.”