Elusive Sjogren's manageable—if diagnosed
Lack of awareness compounds a condition that is exceedingly difficult to diagnose. Experts offer signs and symptoms for ruling it out or diagnosing it more quickly.
A woman in her early fifties comes to her primary care visit reporting an array of symptoms: tiredness despite sleeping nine hours a night, “specks of sand” in her eyeballs, vaginal and skin dryness that she attributes to menopause, and achy joints (“Sort of like a flu that won't go away”). Probing further, her internist notes several cavities in the patient's teeth and slight parotid gland enlargement.
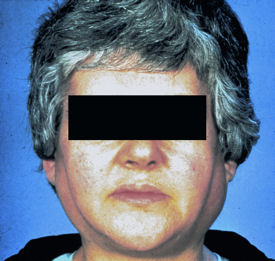
The woman turns out to have a classic case of Sjögren's syndrome, but many internists would miss that diagnosis, said Frederick Vivino, MD, chief of rheumatology at Penn Presbyterian Medical Center in Philadelphia. Even though an estimated 4 million Americans—90% of them women and the vast majority Caucasian—have Sjögren's, “Lack of awareness is a big problem,” he said.
It's not surprising that the disease is often missed, acknowledged Dr. Vivino, chair of the Sjögren's Syndrome Foundation's medical and scientific advisory board. The condition is exceedingly difficult to diagnose. And while it's more common than breast cancer, multiple sclerosis or lupus, its symptoms, such as dryness, are vague, may not occur concurrently, and may not be noticed by patients in the early stages.
Sjögren's often presents like other autoimmune diseases, such as lupus, rheumatoid arthritis and fibromyalgia, and may even overlap with those or other conditions, such as systemic sclerosis. Because Sjögren's frequently afflicts middle-aged women, doctors might attribute its symptoms to menopause. Also, some Sjögren's patients report problems such as peripheral neuropathy, which could mislead doctors to pursue other diagnoses.
Rheumatologist Chris Derk, ACP Member, associate professor of medicine at Thomas Jefferson University in Philadelphia and author of ACP's PIER module on Sjögren's, advised internists to first rule out medications as the culprits in dryness, but to continue workups if patients also have unremitting fatigue and unexplained pain, as well as oral symptoms severe enough to interfere with eating or sleeping.
“Once you start going down that list and looking for other causes and have ruled out hepatitis C, diabetes and sleep apnea, start thinking about Sjögren's,” said Dr. Derk, who practiced as a general internist for four years before going into rheumatology. He admitted that “Sjögren's wasn't on my radar screen then.”
Diagnosing Sjögren's
Because of the vagueness of its symptoms and its similarity to other conditions, it can take as long as eight years for a patient with Sjögren's to receive a correct diagnosis, according to experts and to materials provided by the Sjögren's Syndrome Foundation.
Diagnosis is best approached as a team effort that involves rheumatologists and ophthalmologists, experts agreed. Though it's no simple matter to decide when to pursue and persist in the workup for Sjögren's, Dr. Vivino said, “Sjögren's should be considered in any patient who has persistent dry eyes or mouth, and who has chronic fatigue, or an unexplained chronic muscular condition or joint pain.”
Unexplained dental problems, particularly recurrent caries and possibly periodontal disease, should also raise suspicion, Dr. Derk added.
Robert Meador, MD, a rheumatologist with Baylor Health System in Garland, Texas, serves as advisor to a local Sjögren's support group and the Sjögren's Syndrome Foundation medical advisory board. Dr. Meador, whose practice is made up of roughly 20% Sjögren's patients, acknowledged that a differential diagnosis can be a protracted process because sicca symptoms (dryness of the eyes and mouth) can also occur in hepatitis C and other chronic viruses, hypothyroidism, Addison's and other endocrine diseases, and lymphoma.
Patients who've undergone radiation treatment may also develop sicca symptoms, he said, and the list of possible dryness-inducing medications is long: antihistamines, diuretics, antipsychotics, antidepressants, tranquilizers and some beta blockers.
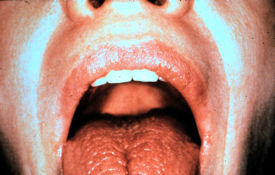
Other physical manifestations that may indicate Sjögren's include a fissured tongue, salivary gland enlargement, blepharitis and frequent bouts of conjunctivitis. Sjögren's patients might, in addition to joint pain and swelling, have sinus tenderness, a purpuric rash and pulmonary crackles. Abdominal tenderness and focal neurological signs may be present as well.
Laboratory and nuclear medicine studies constitute the next step in the diagnostic process. Patients should first be tested for the presence of anti-Ro/SSA and anti-La/SSB and ANA autobodies. If those results are positive—Sjögren's experts caution that 30% of women will test positive—more definitive testing should be pursued. The frequency of anti-Ro/SSA and/or anti-La/SSB antibodies has varied in different studies, but 50% positivity of one or both of these autoantibodies is compatible with most reports of primary Sjögren's patients, Dr. Meador said. Depending upon the methodology employed, and other factors, anti-Ro/SSA antibodies are found in approximately 70% to 97% of patients with primary Sjögren's syndrome. Other key blood tests include rheumatoid factor, sedimentation rate and immunoglobulin levels.
The gold standard in diagnosing Sjögren's is a lip biopsy, used to confirm lymphocytic infiltration of the minor salivary glands. “It's an important diagnostic tool in confirming histologically that it's Sjögren's, but it's also helpful in evaluating severity,” explained Dr. Meador. “Not everyone with Sjögren's requires a salivary gland biopsy for diagnosis, however.”
Indications for salivary gland biopsy include confirmation of a suspected diagnosis of Sjögren's and exclusion of other conditions that can cause xerostomia and bilateral gland enlargement.
The most widely accepted grading system records the number of foci of lymphoid tissue, defined as collections of 50 or more lymphocytes per 4 mm2. Most criteria require more than one focus of lymphocytes per 4 mm2 for a definitive diagnosis, Dr. Meador said.
Before the biopsy is performed, internists may wish to refer patients to a rheumatologist, ophthalmologist and possibly an oral pathologist for evaluation and additional testing. The ophthalmologist (or internist who is comfortable with and proficient at eye tests) will do a Schirmer test to measure tear production. The ophthalmologist performs rose bengal and lissamine green ocular surface staining to look for dry spots caused by dead or dying cells on the eyes' surface. Measurement of salivary flow, salivary scintigraphy (a nuclear medicine test to assess saliva production and glandular function), and parotid sialography (a radiographic dye examination of the parotid ducts) help pinpoint abnormalities of the glands consistent with Sjögren's.
Deciding when to refer in the course of the workup is a matter of personal preference and comfort zone, noted rheumatologist Robert Fox, FACP, PhD, a professor at the Scripps Memorial Hospital and Research Foundation in La Jolla, Calif., who frequently writes about Sjögren's.
But sometimes earlier is better, he advised, if the internist isn't familiar with Sjögren's or if severe xerostomia is present. He cautioned, however, that because of the rheumatologist shortage, it may take a while to have patients seen, and meanwhile, their anxiety level could go up commensurately.
For that reason, Dr. Derk advised internists to approach the referral discussion cautiously and comfortingly. “I would say, ‘We did this [antibody] test, and you're dry, so let's have a rheumatologist look at you,’” he said.
At the same time, Sjögren's patients are often mightily frustrated by the time they get to the rheumatologist's office, Dr. Fox noted, because their symptoms affect their quality of life but haven't been qualified—possibly because they appear healthy. A typical patient may blurt out, for example, “If one more person tells me how good I look, I'm going to hit them,’” Dr. Fox said. “That's because they don't feel good. They feel flu-ish and dry. Their quality of life is diminished.”
Focus on symptoms
The majority of Sjögren's cases are mild and most of the dryness can be well managed topically. For the eyes, alternatives include artificial tears (preferably products without preservatives) and gel-based ocular lubricants to help patients get through the night. Topical cyclosporine 0.05% may be used to treat ocular surface inflammation and improve tear production.
Mild mouth dryness may be alleviated with sugar-free lozenges or special gums. Products that contain xylitol work best and protect against caries. In moderate-severe cases secretagogues, such as pilocarpine and cevimeline, may be needed to stimulate saliva production.
Patients should have frequent dental checkups and consider using topical fluoride and electric toothbrushes. Immunosuppressant drugs are used to treat internal organ or systemic manifestations.
“Sjögren's syndrome is genetically, serologically and epidemiologically comparable in frequency to systemic lupus, and there's a large overlap in clinical features and treatments,” explained Dr. Fox. “But there are some distinguishing features internists should keep in mind, namely the emphasis on topical therapy to address the dry eyes and mouth, and avoiding medications that would exacerbate that.”
However, because Sjögren's is systemic and may, over time, cause corneal or internal organ damage, particularly interstitial disease in the kidneys or lungs, close follow-up and a multi-disciplinary/specialist approach are essential. A chest X-ray is recommended at baseline, as well as kidney and liver function testing and urinalysis. Both Drs. Derk and Vivino voted for having Sjögren's patients see a cornea specialist early on and at least twice annually, for example. “It often takes a cornea specialist to see the damage, and if it's there, more aggressive topical therapy may be needed,” said Dr. Derk.
Even Sjögren's patients with well-controlled, less-aggressive disease should be seen at least quarterly, and should have function of key potentially affected organs assessed through screening tests, experts said. Systemic manifestation affects up to 30% of Sjögren's patients.
“The important thing to realize with Sjögren's syndrome is that it can affect the entire body and can overlap with other autoimmune conditions,” Dr. Meador explained. “So make sure that the organs are monitored for involvement. If you wait for symptoms to arise, the patient could already have significant [organ] damage.”





