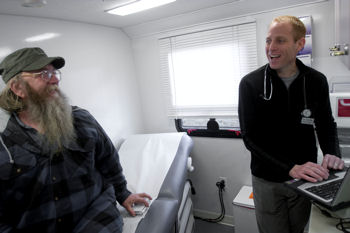
Working toward health care one step at a time
While the presidential candidates debate different strategies for reforming the ailing U.S. health care system, ACP has been quietly working toward change.
While the presidential candidates debate different strategies for reforming the ailing U.S. health care system, ACP has been quietly working toward change. Since 2004, the College has been helping physicians take practical steps toward improving care for patients with chronic diseases through its “Closing the Gap” initiative. The project, which recently wrapped up a three-year phase focused on diabetes care, took an innovative team-based approach to care that has since been embraced by many as a critical pathway to improving physician practice and patient outcomes. The diabetes module resulted in shorter times between visits and more frequent checks of blood pressure, A1c, lipids and urine albumin. More details on the project, which received funding for another two years, are here.
Throughout the diabetes module, funded by an unrestricted grant from Novo Nordisk, teams of doctors, nurses and office administrators were trained in the fundamentals of the Chronic Care Model and how to measure, change and improve the care of their diabetic patients. Bringing medical and administrative staff members together for team training was a first for many participants, and a key to the project's success. Physicians, used to learning in lecture-style CME courses, found they could achieve much more through hands-on sessions that included front- and back-office staff. With other staff members involved in tracking patients' progress, the physician was freed up to focus on patient care. The diabetes project furthers the College's goal of promoting coordinated, team-based care in a patient-centered medical home.
Another longstanding ACP priority is ensuring access to care for the underserved and uninsured. Two articles in this issue look at how enterprising physicians are taking innovative approaches to the problem. Anesthesiologist William Rosenblatt, MD, founded a Web site that links surplus medical equipment in the U.S. to needy recipients in underserved areas. Read Jessica Berthold's “Web Watch” to find out how connections made on Med-Eq led to Iraq amputees getting prosthetics and midwives in Haiti receiving ultrasound machines. Other physicians are taking their primary care skills to the streets, working from converted buses and vans to provide free health care to the homeless. Stacey Butterfield writes about several physicians who travel around their cities in mobile units to bring basic care to a marginalized population.
This issue also includes another diagnostic dilemma in “Mindful Medicine” with Jerome Groopman, FACP, and Pamela Hartzband, FACP, and an ethical case study and commentary by Lachlan Forrow, FACP. Both columns have generated an enthusiastic response from readers. Please continue to send in your comments and ideas.
Sincerely,
Janet Colwell
Editor