MKSAP Quiz: 3-year history of low back pain
A 67-year-old man is evaluated for a 3-year history of low back pain, which is of moderate intensity and worsens during activities, and a 1-year history of neck pain accompanied by 20 minutes of morning stiffness. He reports no radiating symptoms. He has tried ibuprofen, naproxen and acetaminophen, with only partial relief. He also has type 2 diabetes mellitus that is treated with glyburide and metformin.
On physical examination, vital signs are normal. BMI is 34. There is decreased range of motion of the cervical, thoracic and lumbar spine. The patient is unable to touch his toes. Straight-leg-raising test results are normal. There is no tenderness over the sacroiliac joints. Neurologic examination is normal.
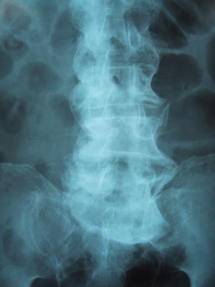
A radiograph of the spine is shown.
Which of the following is the most likely diagnosis?
A. Ankylosing spondylitis
B. Diffuse idiopathic skeletal hyperostosis
C. Lumbar spinal stenosis
D. Spondylolisthesis
Answer and critique
The correct answer is B: Diffuse idiopathic skeletal hyperostosis. This question can be found in MKSAP 16 in the Rheumatology section, item 57.
This patient most likely has diffuse idiopathic skeletal hyperostosis (DISH). He has neck and low back pain and limited mobility throughout the spine. This patient is male, obese and has diabetes mellitus, all of which are risk factors for DISH. This disorder is characterized by calcification of the enthesis regions (where the tendons or ligaments insert into bone) and the spinal ligaments. The diagnosis is confirmed on radiograph by the presence of flowing osteophytes along the anterolateral aspect of at least four contiguous vertebral bodies (most easily detected in the thoracic spine), preserved vertebral height, and absent findings typical for ankylosing spondylitis. Although radiographic involvement of the thoracic spine is characteristic of DISH, this area is often asymptomatic.
Although symptoms of ankylosing spondylitis can be similar to that of DISH, patients with ankylosing spondylitis are typically younger. Furthermore, ankylosing spondylitis demonstrates vertical bridging syndesmophytes, whereas DISH demonstrates flowing linear calcification and ossification along the anterolateral aspects of the vertebral bodies that continue across the disk space. Importantly, sacroiliitis, which occurs in ankylosing spondylitis, is absent in DISH.
Lumbar spinal stenosis leads to chronic low back pain and “pseudoclaudication,” with pain and radiating symptoms down one or both legs that occur with walking and are relieved by rest. The pain is also characteristically relieved by leaning forward as when climbing stairs, walking uphill or leaning onto a shopping cart or walker. Spinal stenosis can be demonstrated radiographically by MRI, showing narrowing of the spinal canal by disks and/or osteophytes.
Spondylolisthesis involves the subluxation of one vertebra over another vertebra. The vertebrae should be in linear alignment. Because of lax ligaments (associated with degenerative disk disease) or damaged ligaments, there can be too much anterior-posterior movement between the vertebrae. Spondylolisthesis can result in nerve root impingement with symptoms of sciatica or chronic low back pain. Diagnosis can be made on plain radiographs of the spine. Findings can be more obvious on flexion-extension lateral views of the spine. This patient's radiographs do not reveal spondylolisthesis.
Key Point
- Diffuse idiopathic skeletal hyperostosis is confirmed on radiograph by the presence of flowing osteophytes along the anterolateral aspect of at least four contiguous vertebral bodies.