MKSAP Quiz: Burning, itching on the mid-back
A 49-year-old woman is evaluated for recurrent burning and itching on her mid-back that have been present for 2 years. She is otherwise healthy, although she does have mild joint aches (neck, lower back, knees) for which she uses ibuprofen intermittently.
Physical examination discloses ill-defined hyperpigmented patches on the mid-back below the medial aspect of the scapulae, as shown. The remainder of her physical examination, including neurologic examination, is normal.
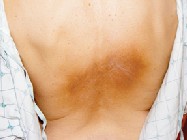
Which of the following is the most likely diagnosis?
A. Herpes zoster
B. Notalgia paresthetica
C. Nummular dermatitis
D. Xerosis
Answer and critique
The correct answer is B: Notalgia paresthetica. This question can be found in MKSAP 15 in the Dermatology section, item 35.
This patient has notalgia paresthetica, which is characterized by recurrent pruritus, burning, or stinging on the mid-back. On physical examination, signs of chronic scratching or rubbing such as hyperpigmentation or lichenification (thickened skin with increased and exaggerated skin markings due to scratching) may be present, but there are no primary skin abnormalities that cause the itching. The skin may appear entirely normal. Notalgia paresthetica and brachioradial pruritus, a similar type of recurrent itching on the forearms, are examples of neuropathic pruritus—itch caused by an anatomic lesion in the peripheral or central nervous system. Some cases of notalgia paresthetica or brachioradial pruritus are associated with disease in the cervical and/or thoracic spine (frequently degenerative changes, such as osteophytes), and radiographic imaging may be appropriate; however, it is unusual to find a cause that would benefit from surgical management. Most patients have a normal neurologic examination despite their intense pruritus. These localized forms of neuropathic itch are difficult to treat; because they are noninflammatory and are not histamine mediated, corticosteroids are generally ineffective, as are antihistamines. Topical anesthetics (such as pramoxine) and topical capsaicin may provide some relief. Successful use of gabapentin, as well as tricyclic antidepressants including amitriptyline, has also been reported. For some patients, clarifying the diagnosis alone can be beneficial.
Herpes zoster presents as pruritic or painful vesicles in a dermatomal distribution. Itching or burning can precede the onset of vesicles; however, this patient's symptoms have persisted for years.
Nummular dermatitis is a pruritic eczematous condition that presents as annular, coin-shaped, erythematous plaques with pinpoint vesicles, overlying oozing scale, and honey-colored, serous crusting. This patient does not have a presentation consistent with nummular dermatitis.
Xerosis is the medical term for dry skin. While dry skin can be itchy, it presents with diffuse flaking of the skin without localized areas of hyperpigmentation. It is most common on the extremities and flanks.
Key Point
- Neuropathic pruritus should be considered in patients with localized itching without associated skin lesions; it can be associated with disease in the cervical and/or thoracic spine.