Anchoring errors ensue when diagnoses get lost in translation
In two cases, a patient's use of key words led to anchoring errors in diagnosing an abdominal aortic aneurism and a classic case of intermittent claudication.
We have discussed errors due to anchoring in past columns. Anchoring refers to the tendency to latch on, or anchor, to the first symptom or bit of data and fail to consider the full spectrum of information, leading to misdiagnosis. Recently, we have received several cases where an anchoring error was triggered by a mistake in translating the patient's words into clinical terms.
Case study #1
Henry Solomon, FACP, currently the medical director of Pfizer Global Pharmaceuticals, was for many years a cardiologist on staff at New York Hospital. He told us about the case of a 65-year-old man from Quito, Ecuador, who came to see him yearly for an “annual physical examination.” The patient, Dr. Solomon said, “was always asymptomatic, and had mild hypertension, mild dyslipidemia, was overweight, smoked cigars, had two drinks per day, and refused to change any of these behaviors or take any medications.”
Several months before his usual time to visit New York, the patient was lying prone on the beach, and felt his body slowly rising and falling. Thinking it might be a small earthquake or ground tremor, he looked around to see if others were similarly aware of such motion, but nobody appeared to be. The patient said he turned on to his back and the feeling stopped. Rolling again onto his belly, the feeling returned. The patient called his local physician who dismissed the symptom as “gas.”
The local physician, hearing what was clearly an unusual description of abdominal symptoms, was faced with the task of translating the patient's complaint into clinical terms. Certainly, patients use all kinds of descriptors to refer to “gas,” such as rumbling, grumbling or squeezing. Furthermore, “gas” is used as an explanation for a variety of transient minor abdominal symptoms that are of no consequence and, in fact, may not be due to “gas.” Thus, it is not surprising that the local physician anchored on this diagnosis.
But, the patient felt the sensation was so unusual that he called Dr. Solomon in New York. Dr. Solomon elicited further history that the patient felt his body was literally rising and falling in a gentle rhythmic way while lying on his abdomen. The feeling went away as soon as he turned onto his back. He did the experiment three times and each time his symptoms were the same.
“As I mentally went through differential diagnoses,” Dr. Solomon said, “I couldn't shake the idea that this could possibly be a large abdominal aortic aneurysm. When I explained my concern to the patient, repeating that this would be a rare and unusual presentation, I said that the seriousness of the possibility made immediate medical attention necessary. Against my every entreaty, he insisted he would fly to New York immediately. I explained the dangers of flying with that condition, that reduced cabin-air pressure could be disastrous, that immediate care was essential, but he ignored it all and said that he was coming to New York.”
Unable to dissuade the patient, Dr. Solomon said that he “arranged for immediate transport to the hospital from JFK International Airport and within two hours of arrival—fortunately he arrived intact—the patient was in the operating room where a huge, bulging, pulsating abdominal aortic aneurysm was successfully treated.”
Commentary
Dr. Solomon told us that he loves language. In this case, he took the time to really think about the patient's words and to run through a differential diagnosis. He was able to translate the patient's description and thereby arrive at what turned out to be the correct etiology, avoiding the anchoring error.
This patient presented with an unfamiliar description that was misleading to the local doctor. But sometimes even familiar descriptions can mislead a physician and lead to anchoring errors because the same words may have different meanings for the patient than for the doctor.
Case #2
Arthur Chernoff, ACP Member, chief of endocrinology at Einstein Medical Hospital in Jenkintown, Pa., shared with us the case of an 80-year-old man who required knee surgery for arthritis that severely limited his ability to walk. After surgery and rehabilitation, the patient was able to walk and ventured out on the golf course for the first time in several years. However, he reported that he was “fatigued” and had “no stamina.” The orthopedic surgeon referred him to his internist who sent him to a cardiologist.
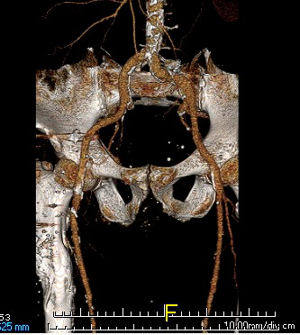
An extensive evaluation showed normal pulmonary and cardiac function. The patient, having seen advertisements for testosterone therapy, said to his internist, “I hear testosterone can help your stamina,” and asked that he check his testosterone level. The internist complied and found a level of 242 ng/dL (where 240 was the lower limit of normal) and referred him for an endocrine evaluation.
Dr. Chernoff questioned the patient regarding libido and sexual function, and was told, “In this area, things are great.” Dr. Chernoff then said to the patient, “I want to hear in your words about the problem.” The patient replied as he had done before, “I have fatigue and lose stamina.” At this point, Dr. Chernoff said, “What do you mean by fatigue and lose stamina?” The man replied, “Whenever I walk, I lose stamina,” pointing to his calf. “When I stop walking, the stamina comes back and I can walk again.”
Dr. Chernoff told us, “It was a classic description of intermittent claudication.” On physical examination, a loud right femoral bruit was easily heard. Dr. Chernoff referred the patient to a vascular surgeon, and a successful angioplasty was performed. “The man is now back on the golf course,” Dr. Chernoff reported.
Commentary
It is easy to see how a physician could be misled by the words this patient used to describe his symptoms. It took an extra step to determine exactly what the patient meant by “fatigue” and “stamina.” Part of being an effective physician involves functioning as a translator of the patient's symptoms, converting the patient's words into human biology. Mutual understanding between doctor and patient is essential to ensure accurate diagnosis and appropriate medical care.
Dr. Chernoff concluded his description of the case as follows: “The reimbursement for the correct diagnosis: $. The reimbursements for all the unnecessary testing prior to the correct diagnosis: $$$$. The satisfaction in getting it right … priceless.”


