Mindful Medicine: Don't let emotion impede right diagnosis
A case study shows how affective errors can lead to a missed diagnosis, by Jerome Groopman, FACP and Pamela Hartzband, FACP.
Moshe Chasky, ACP Member, a senior hematology/oncology fellow at Fox Chase Cancer Center in Philadelphia, contacted us about a case of a 50-year-old man with chronic lymphocytic leukemia (CLL) referred to the hematology clinic for a second opinion. The patient was a photographer but for the past eight years had been on disability for chronic pain, headaches and anorexia with a diagnosis of fibromyalgia. He had seen five rheumatologists and was receiving high doses of morphine (MS Contin) from his primary care doctor to control his pain.
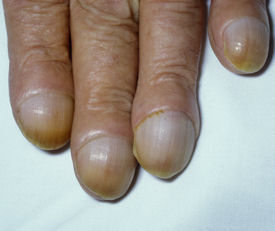
On physical examination, Dr. Chasky noted that the man “had a ruddy complexion and obvious clubbing of his fingers. I was trained at Sackler Medical School in Tel Aviv, where there was a tremendous emphasis on physical examination,” he said. “One of my mentors insisted on careful study of the hands.”
The patient had no splenomegaly or lymphadenopathy. Pulse oximetry showed an oxygen saturation of 95% on room air. Laboratory data included:
- elevated hemoglobin of 17.5 g/dL
- minimally elevated lymphocyte count
- normal platelet count
- negative Jak2 mutation test
Commentary: Review the history
Dr. Chasky said he concluded that the patient did have CLL, and that there was no indication for therapy. But he saw how miserable the patient was and wanted to help him in some way. He wondered whether the physical finding of clubbing and the laboratory result of erythrocytosis with mildly decreased oxygen saturation—disproportionate to the increase in red blood cells—could be related to his chronic symptoms and diagnosis of fibromyalgia.
Upon querying the patient further, he learned that his symptoms had begun after he moved to a new house eight years earlier. Dr. Chasky also learned that the patient smoked two to three cigars a day, generally while working in the basement of the new house where he had built a darkroom.
Dr. Chasky obtained an arterial blood gas with cooximetry which revealed an elevated carboxyhemoglobin of 13.2%. The patient was instructed to obtain a carbon monoxide detector. Readings in his house and basement were normal. Dr. Chasky wondered whether smoking several cigars in a closed space like the darkroom could result in elevated CO levels, so he asked the patient to stop smoking. Subsequent testing showed a decrease in the carboxyhemoglobin levels to 10% after four days and to 4% after three weeks. In addition, the patient was evaluated for sleep apnea and was treated with continuous positive airway pressure. With these interventions, the chronic pain, headaches, anorexia and other symptoms that had been entirely attributed to fibromyalgia improved markedly and he was able to reduce his pain medications.
Emotions influence diagnosis
We have commented previously on the issue of “diagnosis momentum,” the problem of passing on a diagnosis from doctor to doctor so that it becomes fixed and unquestioned. In this case, the patient had seen five specialists, each confirming the diagnosis of fibromyalgia. This patient may well have had fibromyalgia but also had an additional condition causing similar symptoms.
Fibromyalgia is difficult to diagnose because it depends on clinical symptoms and patient reporting of discomfort during palpation of at least 11 of 18 tender point sites. There is no confirmatory objective laboratory test, distinctive imaging abnormality or pathologic finding on biopsy of muscle or nerve. In the past, syndromes like fibromyalgia were termed “wastebasket diagnoses,” a pejorative appellation referring to symptoms that cannot be confirmed by objective anatomical or biochemical abnormalities. Recently, the FDA approved pregabalin (Lyrica) for treatment of fibromyalgia. Although this is an advance in therapy for patients suffering from the condition, ironically the availability of a treatment may contribute to incomplete evaluation for secondary causes of symptoms that may mimic fibromyalgia.
Patients with fibromyalgia and other chronic pain syndromes have often seen multiple physicians, are taking narcotics and express disappointment with the medical profession. These patients can evoke a sense of failure and frustration in the physician.
In our experience, a major contributor to diagnosis momentum in this kind of patient is what psychologists call “affective error,” a term used to describe thinking blurred by an emotional reaction. In How Doctors Think, Donald A. Redelmeier, FACP, an internist at the University of Toronto who has studied physician cognition, elaborated very frankly about the negative emotional reactions many physicians have to patients who do not care for themselves, such as alcoholics or drug abusers.
Many of us have read the article by J.E. Groves, “Taking care of the hateful patient,” in which he describes patients who cling, demand, manipulate and/or engage in self destructive behavior, stimulating negative feelings in their doctors. (NEJM 298 [1978], pp. 883-887). Debra Roter, PhD, professor in the department of health, behavior and society at Johns Hopkins Bloomberg School of Public Health, and Judith Hall, PhD, professor of social psychology at Northeastern University, have studied the effects of such negative attitudes toward patients and found that they can blunt effective communication and impair optimal care (“Liking in the physician-patient relationship,” Patient Education and Counseling 48 [2002], pp. 69-77.)
When the emotional reaction is severe, we recognize it. But we may not appreciate more subtle emotions that can nonetheless influence our thinking. Patients who trigger a negative emotion in the doctor may be too readily moved out of the office, prescription in hand, without a thorough evaluation.
In the case described, Dr. Chasky was not detoured by an affective error in his thinking, nor was he overcome by diagnosis momentum. “My assessment was that the CLL was indolent and almost an incidental finding,” Dr. Chasky told us. “The more interesting problem was his fibromyalgia and his clubbing.” Dr. Chasky's attitude reflects an open and questioning mind that is not deterred by negative emotional influences, and is crucial to being an effective diagnostician.




